Two days ago, I wrote about the need to assess COVID risk for loved ones who reside in nursing homes. For many people, it has been impossible either to remove or even to see their family members in these facilities.
Clearly, nursing homes are one of the largest sources of coronavirus deaths as it has been estimated that almost 1/3 of the US COVID deaths came from these facilities. What was not clear was whether elderly people in these facilities were at risk simply because of their health status or were at increased risk because of their presence in nursing homes.
An analysis from the Centers for Medicare and Medicaid Services released yesterday and data from two new studies provide one of the first organized assessments of COVID-19 infections and deaths in nursing homes. While many of the insights provided reinforced general concerns about these facilities, looking specifically at different types of nursing homes did give new and unique insights into what may be at play with these infections.

THE CMS survey of nursing homes, showed 25,923 resident deaths tied to Covid-19, the disease caused by the virus, and 449 deaths among the facilities’ staff. The survey also found about 95,000 infection cases at nursing homes across 49 states, about a third of them among staff members. But a Wall Street Journal analysis suggested these numbers underestimated the problem.
The May 8 CMS rule that mandated reporting of nursing home COVID statistics didn’t require reporting of deaths and cases that occurred before early May. Also, assisted-living facilities not regulated by CMS were not required to submit any information, though they could do so voluntarily.

Despite this concern, CMS Administrator Seema Verma said in the Wall Street Journal the agency believed that the “vast majority” of nursing homes had in fact provided data from before May 8. CMS did say about 20% of 15,400 nursing homes had not reported the required data by May 24.
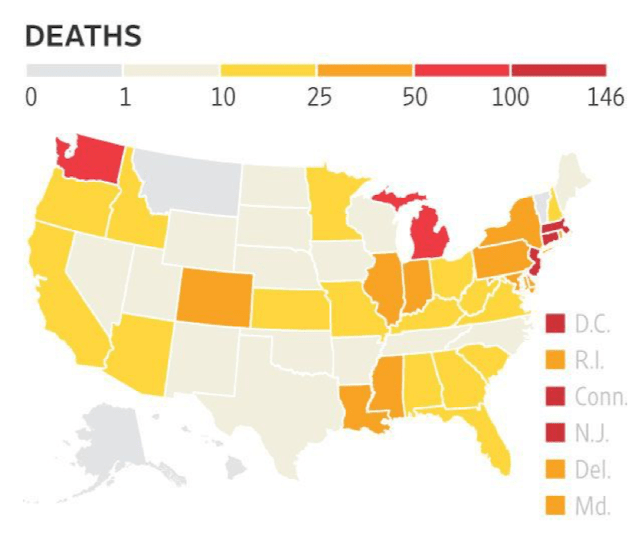
In contrast, a WSJ tally of state data from around the U.S. shows more than 42,000 Covid-19-associated deaths in long-term-care facilities, including nursing homes and assisted-living sites, along with more than 200,000 cases. The Journal believed even this number likely undercounts numbers because of reporting lags and incomplete information from some states.
Given that approximately 104,000 deaths nationwide are now linked to Covid-19, nursing homes are providing 40% of that total.
Trying to identify whether there are facility related factors related to COVID-19 cases in nursing facilities has been difficult. Two new studies highlighted in Forbes and reviewed in Provider Magazine, examined which factors are associated with cases of Covid-19. An analysis by David Grabowski of Harvard University, using data from 20 states, found that the factors most clearly linked with facilities having a Covid-19 case included being in states with significant spread of the virus, an urban location, and a greater share of African American residents. Being a for-profit nursing home was associated with having larger outbreaks, the analysis found.
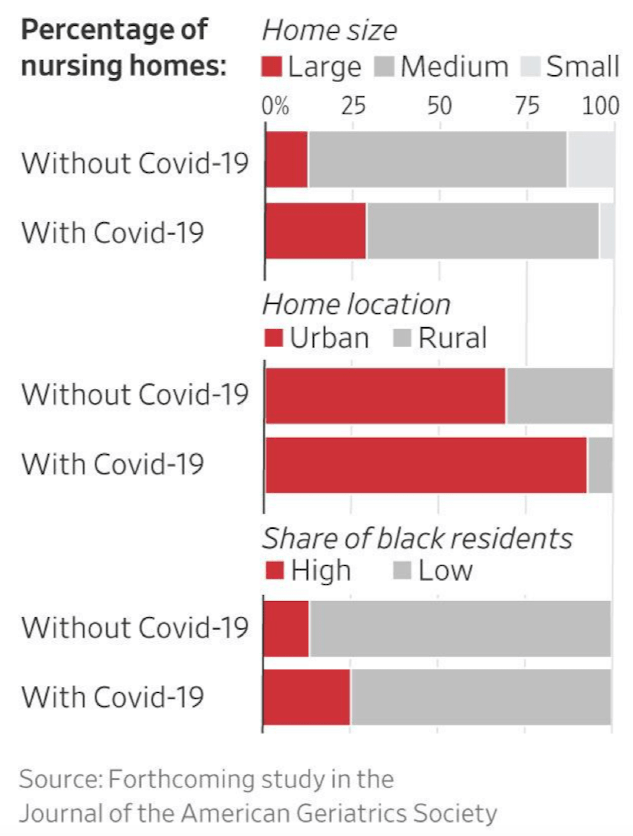
Of interest, these analyses also tell a surprising story: quality (at least as measured by Medicare), the percentage of Medicaid residents, and a facility’s business model don’t indicate whether a facility is likely to have an outbreak.
This was reinforced by preliminary research from Vincent Mor, PhD, professor, Florence Pierce Grant University. He states that “it’s a function of traffic; that is, if you’re in an environment where there are a lot of people in the community who have COVID, the patients in the building are more likely to have COVID. It’s as important.” He added, “If you are a larger facility versus a smaller facility, there is more traffic. Larger facilities simply have more staff, more people coming in and out of them. That’s more traffic and more likelihood that someone will be coming in from the outside with COVID.”

Thus, while nursing facilities clearly are a major source of COVID infections and deaths, they remain more of a reflection of their communities than an isolated environment. Importantly, while there are factors associated with increased risk that appear to be related to the home, there is no absolute way to identify a suspect facility. CMS will be publishing the individual data soon so you can check specifically on your loved one’s facility.