As if I had predicted it in my blog yesterday, a new paper just published suggested that the immune response to coronaviruses could be very long lasted, as long as 17 years. This peer reviewed publication in the prestigious scientific journal Nature looked at cellular immune responses in three groups of individuals who had been infected with either COVID-19, SARS, or neither of the viruses. Their conclusion was that cellular immunity could be very long lived; in the case of SARS almost 17 years since the epidemic occurred in 2003.

In addition, this study disclosed evidence of cross-reactive immunity to SARS-CoV-2 in individuals infected with SARS, and even found evidence of cellular immunity to the COVID-19 virus in individuals who had not been infected with either virus. The implications of these finding are important, as they suggest there is long lasting immunity to COVID-19 infection, and this type of immunity may already be present in our population regardless of the presence of antibody against the virus.
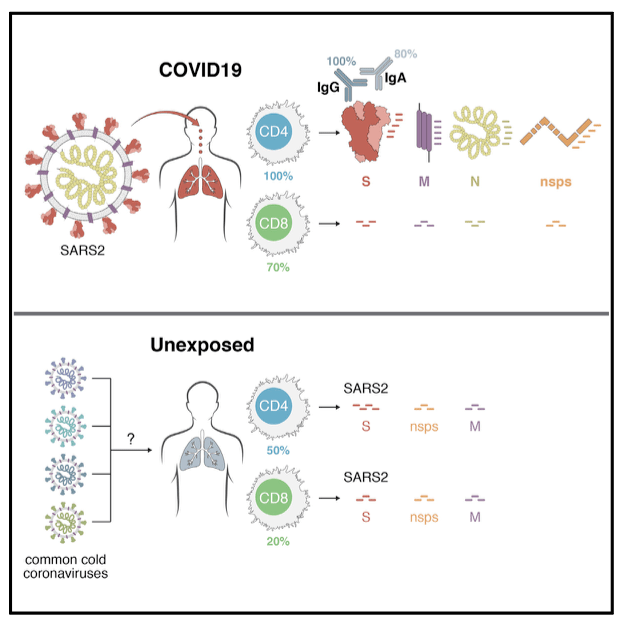
The study led by Duke-NUS Medical School, in Singapore, evaluated 36 individuals who had been infected with SARS-CoV-2, 23 patients infected with SARS in 2003, and 37 volunteers who had not been infected with either virus. The subjects were evaluated for T cells that could recognize and mobilize an immune response to the virus.
T cells are the long-lived memory of immunity to a viral infection. They can produce antiviral hormones, activate the production of new antibodies, and directly kill virally infected cells. The lifespan of these memory cells is unknown, and the authors wanted to determine if they were present short term in COVID-19 infected patients. They also wanted to know if patients infected with SARS in 2003 had T cell memory 17 years later, and whether it might recognize SARS-CoV-2 virus that causes COVID-19. They also wondered if patients without an infection to either virus might recognize SARS-CoV-2 through other, “common cold” coronaviruses.
The answer to all these questions was a resounding yes! All the recovered COVID-19 patients had strong T cell memory immunity, and these cells had activity against multiple virus proteins. Most of the SARS patients had detectable anti-SARS immunity 17 years later, and all of the patients produced cross-reactive T cells that could recognize multiple SARS-CoV-2 (the COVID-19 virus) proteins and kill the virus.
Remarkably, even 19 (50% of the 36) individuals never infected with either virus were able to recognize SARS-CoV-2 and produce protective immunity. The authors believe these T cells may exist due to previous infection with another coronavirus, of which there are seven that can infect humans. This reinforces earlier work from the La Jolla Institute for Immunology showing T cell immunity for COVID-19 from other coronaviruses.
This information documents long lived immunity to coronavirus after infection. It should put to bed the concept that people will only be protected for a few months, and then only based on the presence of antibody. Antibody is a useful marker to identify infected people and as a documentation of the presence of an immune response. However, the T cell is the master of the immune response, and if SARS-CoV-2 reactive T cells are present, we have protective immunity.
Now we can focus on inducing an immune response that protects our population. It will be a race between herd immunity and a vaccine.
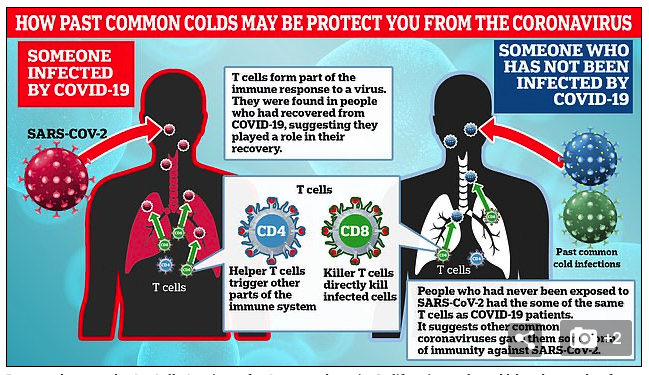
So, if there are people with immunity to Covid-19 based on previous exposure to other coronaviruses, could this partially explain the wildly different outcomes to exposure/infection? That would be good to know. Obviously.
Right now the virus is Russian Roulette because, if even if you are healthy with no comorbidities, you are still taking a chance on death or long term damage if you are exposed. But if we could be more granular about who is and is not at risk, based on pre-existing immune reactions, that could help quite a bit.
LikeLike
I think doing a study to examine if preexisting cellular immunity is protective would be important. I disagree, however, that the virus is “Russian roulette.” Almost every person (>95% in studies from NYC and Washington State) of individuals who have died have had a co-morbidity, especially morbid obesity, type 2 diabetes or cardiovascular disease. If a person has those risk factors they need to show extreme caution.
LikeLike
So ?? Is this wrong ??
https://www.sfchronicle.com/health/article/With-coronavirus-antibodies-fading-fast-focus-15414533.php
LikeLike
I could not read more than a paragraph since I am not a subscriber, but yes it appears it is wrong.
If one had a vaccine only based on antibody, it would not last very long. But that would be an unusual vaccine and would not be a provide good protection to begin with. Most effective vaccines induce not just antibody but cellular immunity, which would be long lasting.
The reason many approaches to vaccines are being funded is that some may not be strong, but others will induce cellular immunity and be fully protective for several years at the least.
LikeLiked by 1 person
If increased Covid resistance as the result of a recent cold is suspected, would it make sense to imagine a voluntary program that would include exposure to a weaker corona-virus. Maybe an induced October cold could offer protection against contracting Covid-19 in the winter, when the annual flu season impacts hospital capacity.
LikeLiked by 1 person
Dr. Baker, I had Covid in July. I had a pretty intense case complicated by asthma. I fortunately had a nebulizer and did not have to go to the hospital. I have been told over and over I can get it again. I knew that I could not, but could not verify it on my own. My doctor told me about your blog and this particular post. I cannot tell the relief to read this and share it with my family and others who will be receptive to truth. Fear is a addictive and a liar. I wish people would turn off the constant stream of fear on their TV. sigh, Anyhow, thank you so much for your blog. It brought such comfort to me. I have other questions for you. Is there a way I can ask them of you?
LikeLiked by 1 person
I am happy you are better. Just ask your questions via the email link.
LikeLike