I had to reschedule Biscuit’s latest message tonight in order to address a more pressing issue. Three days ago, I wrote about the FDA’s refusal to approve convalescent plasma infusions as a treatment for COVID-19. This afternoon, the FDA seemingly reversed itself and provided Emergency Use Approval (EUA) for using this approach to treat individuals acutely infected with COVID-19.
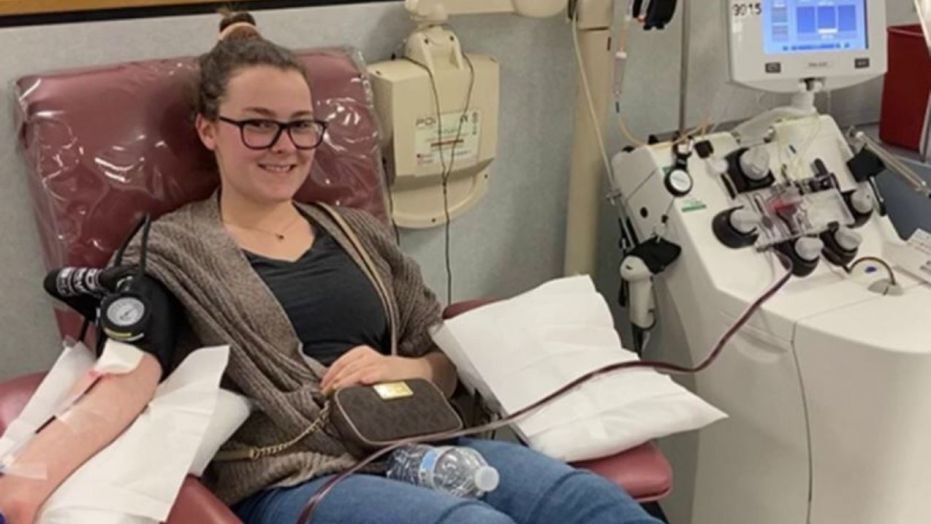
This approach involves harvesting blood plasma (liquid) from individuals who have successfully recovered from COVID-19. The plasma contains antibodies against the virus, which are then pooled and injected into the vein of individuals who are acutely infected with the virus. The theory is that the antibodies neutralize the virus and help infected individuals recover.
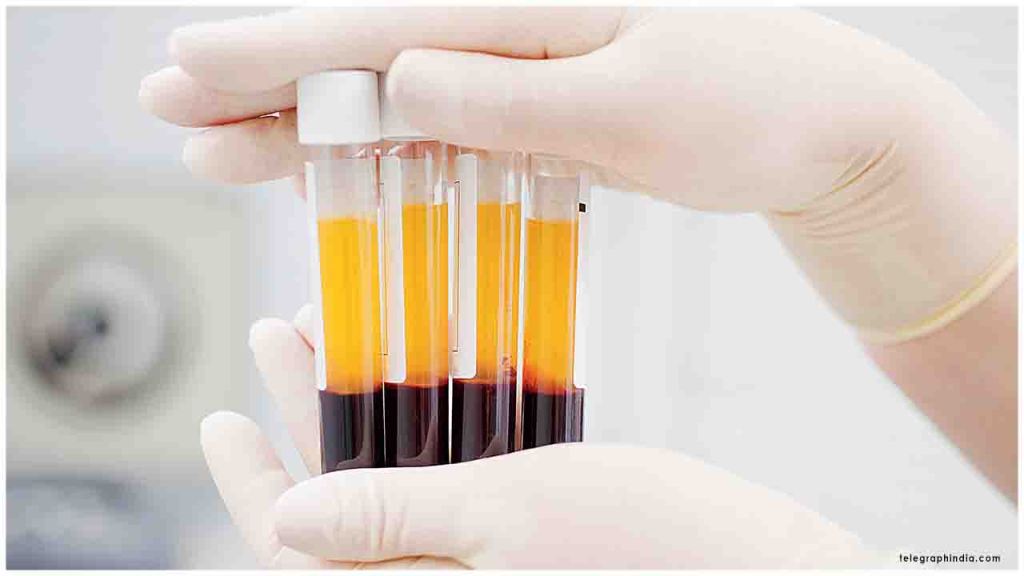
The FDA had reviewed the data associated with these plasma transfusions and found it to be less than compelling or convincing. Despite this, today they gave the approval for EUA status allowing it to be used more widely for COVID-19 patients.
A large study published on Aug. 12 by a consortium of investigators who first conceived of the therapy showed value in reducing mortality. They found that transfusion of convalescent plasma with more COVID-19 antibodies to hospitalized COVID-19 patients significantly reduced mortality compared to transfusions with less COVID antibodies. The definition of more vs. less COVID-19 antibody seemed arbitrary. Transfusions within three days of COVID-19 diagnosis yielded greater reductions in mortality.
This study, however, was not peer-reviewed and importantly did not include a control group that would have allowed the researchers to determine whether the plasma treatment reduced the risk of death when compared to standard care. Also, breaking down endpoints by secondary standards, such as antibody titer, should be done before the study is started, not during the analysis.
Another of the positive studies, by researchers at Houston Methodist hospitals, showed that 136 patients who received infusions of convalescent plasma were more likely to have survived a month post-diagnosis as compared to 251 patients who did not get the treatment. The effect was strongest in people who were given plasma within three days of hospital admission. But the study, published on August 10 in the American Journal of Pathology, was not randomized or controlled. The doctors running the study gave every enrolled patient plasma, and later compared their outcomes to other people treated at the hospital.
In contrast, data from the only two controlled trials the FDA identified in the FDA’s emergency use authorization, failed to show benefit and were stopped. One trial in China could not enroll enough patients. A Dutch trial ended after sponsors found “no difference in mortality, hospital stay or day-15 disease severity.”
This may be an interesting parallel to hydroxychloroquine where uncontrolled studies showed benefit while definitive, controlled studies did not. However, without controlled studies no one can say. This is not something that is permanent as hydroxychloroquine had its EUA withdrawn after definitive studies were published showing a lack of value.

Dr. Stephen Hahn, head of the FDA, gave no insight into the reversal. Janet Woodcock, the head of FDA’s drug division, who is now working on Operation Warp Speed, an interagency effort to accelerate coronavirus treatments and vaccines, was quoted by POLITICO on Friday as saying that plasma has not been “proven as an effective treatment.” In contrast, there was a mixed reaction in the medical community to the EUA, with many believing that the therapy was potentially beneficial and not dangerous for patients. Almost everyone, however, wanted definitive data showing true benefit to patients from controlled human trials. Animal studies do not suggest this will be an effective treatment as I explained three days ago.
The real concern is that wasting time and resources on an expensive and cumbersome therapy like serum transfer will take away focus from finding effective treatments, and this could result in more COVID-19 deaths in the long run.
One thought on “Emerging news story: FDA reverses itself on plasma transfusions for COVID-19”