
One of the first questions people asked when they found we had effective vaccines available was when the public health restrictions on our lives could be removed? This particularly focused on social distancing, mask wearing, and closing of restaurants and other businesses.
I have watched with some frustration many of the news commentators making it sound as if social distancing will go on forever regardless of the vaccine. This is in part because many of these commentators do not have either credentials or background to understand the dynamics of immune protection in a pandemic. But even some of the physicians, notably Dr. Gupta on MSNBC, seem to just rant about keeping these public health restrictions in place indefinitely.
Clearly, during the early days of the vaccine rollout, we cannot reduce social distancing or masking, but we need to have some type of reasonable plan going forward to understand when we will be able to get on with our lives. In order to do this, we need to understand what large scale vaccination can offer in ending the pandemic.
Again, this goes back to “herd immunity,” which unfortunately has become a hot button in the culture wars, and is misused on both sides of the pandemic debate. I will not get into the argument about trying to achieve herd immunity through natural infection. In fact, we should stop arguing about this entirely since we now have a faster and safer method of achieving herd immunity — that is vaccination.
The basic concept underlying herd immunity through vaccinations is that once enough individuals have immunity to the infection, it becomes exceedingly hard to transmit. Infected individuals are few and far between while susceptible, non-immune hosts are rare. So basically, there are so few people to spread the infection that it dies out. That is when the more onerous public health restrictions can end.
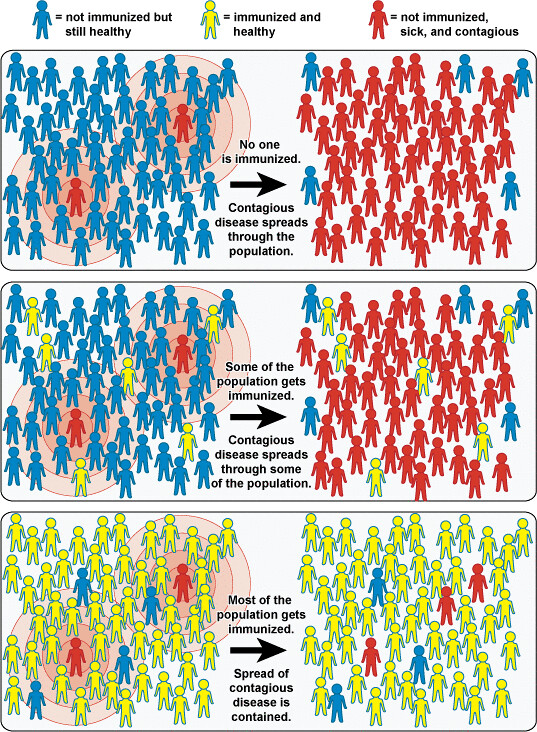
The question is, when do we achieve herd immunity? That is determined by a couple of factors, one being the ease of spread of this respiratory virus and another the degree of protection the vaccine provides. We know that this virus is relatively easy to spread, albeit the specifics of this spread are not fully defined. The very good news is that the RNA based vaccines appear very effective (95%) for preventing symptomatic or severe COVID-19. The Moderna vaccine results also suggest it prevents asymptomatic infection. Therefore, the ease of transmission of this virus is somewhat offset by the high efficacy of the vaccine.
Given these parameters, the conventional wisdom from the public health community has been that you need approximately 70% of the population immunized before you can think that you have herd immunity. This number has also been proffered by Dr. Fauci. There could be significant modifications to this, as I will outline below, but it serves as a good target to begin conversations.
Given the number of current doses of vaccine that are reported to be available to the United States, herd immunity could be achieved sometime in the middle of this coming year. Alex Azar, Secretary of Health and Human Services, has stated that by June anyone who wants vaccine will have it available. So, if everyone is aggressive in getting vaccinated, 70% immunity could be achieved before the fall.
It may also be that we do not need 70% immunization rates to achieve herd immunity. Immunity from COVID-19 infection appears to be effective (at least for a time) in preventing reinfection, so these individuals could be included in the 70%. Also, some individuals appear to have protection through cross reactive immunity, potentially from other coronavirus infections. Further, we are beginning immunizations with those individuals who are most likely to become ill, hospitalized, or die from this infection. Once these individuals are protected, the need for social restriction to prevent the devastating effects of COVID-19 on the medical system may be much less. Together, this may mean that herd immunity will be achieved earlier than we think.
However, many things can delay achieving herd immunity over the next year. Enough vaccine may not be available to vaccinate 70% of the population. Also, the vaccine may not be as effective in the long term as it currently appears. That might mean vaccinated individuals would become susceptible to infection and start spreading the infection again before we could immunize 70% of the population. But the biggest risk to achieving herd immunity is people refusing to be vaccinated. Those individuals will serve as a reservoir to keep COVID-19 spreading. If we do not keep infections down in the next six months, our health system could become dysfunctional to the point that vaccination efforts would be disrupted.
If all goes well, life could be very much back to normal by next fall. However, there are many risks along the way. The good news is that we will be able to tell how we’re doing in real time by monitoring the numbers of COVID-19 hospitalizations and clinical infections. When they drop precipitously we will be nearing our goal!
How does the alleged new strain of the virus in London affect the rate of herd immunity and effectiveness of the currently available vaccines?
LikeLiked by 1 person
Will discuss the London strain tomorrow.
Best, Jim
LikeLike