I received a very strong response to the first part of my discussion about how RNA vaccines work. However, several people wanted more information particularly on why an RNA vaccine would be better or different from a protein vaccine. The comment below was typical.
“Why screw around with mRNA (rife with technical difficulties even if brilliant) and causing the body to make its own viral proteins, instead of just directly injecting those? Would the dendritic cells and rest of the immune system not react the same way? It’s not that the mRNA lasts longer… All I’ve heard is that it’s easier to produce the necessary (though still tiny) quantities of mRNA compared with viral proteins, for some reason. Can you please explain that?
RNA vaccines are harder to store and transport than protein vaccines, so that is actually a disadvantage for their use. However, the value of RNA vaccines for COVID-19 is not just ease of manufacturing. They have an inherent advantage over protein vaccines for this particular infection. This is not clear to many people, but is important to understand. Therefore, I will attempt to explain this complex (warning) advantage and describe how the immune system recognizes foreign invaders in the body.
The immune system has sentinel cells, macrophages and dendritic cells, located throughout the body. These cells are the sensors which identify any foreign invader and its potential as a danger to you. These cells have receptors for different types of materials that are unique to infectious agents. The receptors are called pathogen-associated molecular pattern molecules (PAMPs) and identify structures specific to different types of infectious agents. When they sense these materials the cells activate your immune response to clear the infection (before it can harm you).
The microbial molecules recognized by PAMPs have different general “patterns,” or structures, that alert immune cells to destroy intruding pathogens. They might, for example, recognize one type of lipid shared by bacteria or the genetic material (DNA or RNA) from a group of viruses. This is different from antibodies and T cells, which recognize only proteins from only one type of infectious agent in a very specific manner.
The key point to understand is that proteins alone usually don’t induce danger signals that activate the immune system. This prevents things like autoimmune disease but means that protein-based vaccines need some type of additional material to activate the immune system. Protein vaccines are therefore mixed with some type of inflammatory material called an adjuvant that activates an immune response to the protein.
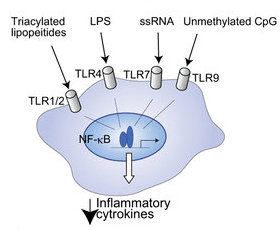
An example of this is the Novavax COVID-19 spike protein vaccine which requires a lipid adjuvant to induce an immune response to the protein. In contrast, the RNA COVID-19 vaccines do not need an adjuvant because the RNA itself activates receptors in dendritic cells thereby inducing an immune response to the spike protein the RNA makes the cells produce.
Since COVID-19 is caused by an RNA virus, the RNA based vaccines activate the immune system in exactly the same manner as the virus. In this way they are uniquely marshaling the immune response to protect from an RNA virus infection. This type of vaccine, however, may not work as well in a vaccine for a DNA virus or bacteria.
Therefore, as compared to protein vaccines, RNA-based vaccines are uniquely effective in protecting against RNA virus infections.