There has been a lot of talk about having to create new vaccines for every different COVID-19/SARS-CoV-2 variant. This assumption is based in part on the fact that influenza vaccines have to be made uniquely every year for whatever types of influenza virus are present in the population.
Recent research from the National Institutes of Health and the Yerkes National Primate Center in Atlanta shows that booster Moderna vaccines made to uniquely match the spike protein of the Omicron variant were no better (or worse) than the current Moderna vaccine in producing immunity or protecting from Omicron infection.

Of interest, this type of efficacy for the initial vaccine against new variants was previously seen with the Beta variant, but scientists thought a variant-specific vaccine might be better in this case because Omicron has many more differences in structure than the initial SARS-CoV-2 virus for which the current vaccines were developed.
The finding that current vaccines are highly effective at preventing infection to SARS-CoV-2 variants is very good news. If over the next few years our immunity wanes (the speed of this is not known) and a new variant develops, we won’t need to go through the development cycle of an entirely new vaccine. The development cycle for mRNA vaccines is relatively short, but the current results suggest we will be able to stockpile vaccine to get a head start on any future COVID outbreak.

The reason the vaccines are so effective against the many SARS-CoV-2 variants has been debated. Some believe it is the result of something referred to as the “original sin” of immunity. This is simply explained as you always respond better to the first antigen you are exposed to. Thus, the immune response to the original COVID vaccine meant these animals would respond better to a boost with that vaccine. However, this theory does not explain the high efficacy of the Omicron booster, which would not be as effective if hampered by “original sin”.
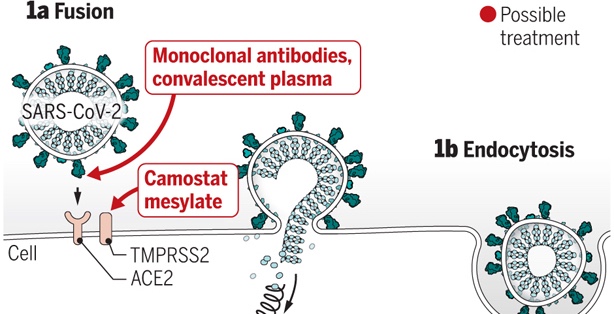
I don’t agree with this concept and believe this result is due to an important difference in how Influenza and COVID-19 viruses infect humans. Both viruses infect by binding like Velcro to human cells, with multiple identical interactions between proteins on the virus and molecules on the membranes of human cells.
But influenza binds to sugars on the surface of human cells. These sugars are coupled to many different proteins, so influenza viruses can bind to almost any cell in the body. Influenza can change its target human binding protein to escape immunity, but still infect humans because it binds to the sugar. For example, bird flu is very dangerous, but only binds to gastrointestinal cells. It doesn’t bind to nose or lung cells, so we don’t have respiratory pandemics of bird flu (yet).
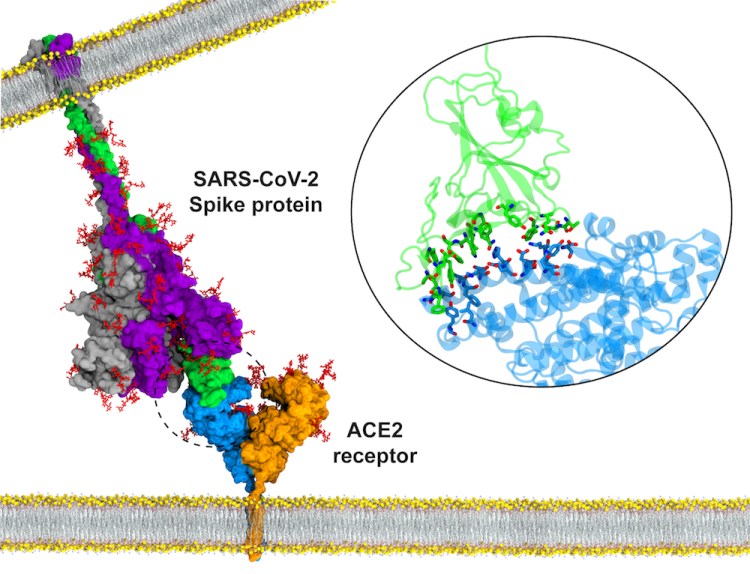
In contrast, SARS-CoV-2 binds to only a single protein; human ACE2. This is a very specific interaction, and if the virus spike protein (which is the vaccine component) changes too much to escape immunity, the SARS-CoV-2 cannot infect humans.
So the incredible infectivity of the COVID-19 virus caused by this very unique protein interaction may also be the Achilles heal that allows us to develop long term immune protection.
Dr Baker,
Your blog is wonderful and has been a reliable source of information. Thank you!
If you have the interest or time available, I’m wondering if you could help me understand why some diabetics’ numbers went up after receiving the vaccine. What is the connection?
Thank you!
LikeLiked by 1 person
Anything that causes inflammation csn increase blood glucose. Luckily the vaccine much less than COVID.
LikeLike
Thank you Jim and best wishes. Last night the news reported that there is evidence from Israel and Britain that the third shot (booster) wanes after 4 months and “a fourth shot may be recommended for the more vulnerable”. In today’s presentation, you imply that this waning of the booster is still unknown. As a 73 year old, should I get a 4th shot before I travel to Mexico next week? I received my booster 6 months ago. Thank you. Randy
LikeLiked by 1 person
Also, in SC for 5 days if you can come to Seabrook for golf on Tuesday. Will try yo get reid as well.
LikeLike
Hi Randy. Good to hear from you. Short answer is no. The data from those studies has not been validated and more extensive work suggests a 4th booster doesn’t help. Protection from death and serious illness does not wane. Best. Jim
LikeLike