The United States has new COVID-19 booster vaccines available for administration this fall, and they are different from the original mRNA vaccines. How these vaccines differ from their predecessors and who would be most helped by getting these boosters are incredibly important questions. I hope to answer these and other questions in this blog post and resolve what has become a remarkably confusing topic!
- What are the new booster vaccines?
The new boosters are mRNA vaccines almost identical to the original formulations from Moderna and Pfizer/BioNtech (see figure). The difference is that rather than containing only the messenger RNA for the original Wuhan COVID virus spike antigen, they also contain the messenger RNA for two Omicron viruses: BA4 and BA5. Despite this, the total amount of RNA and all other components of these boosters is identical to the original vaccines.
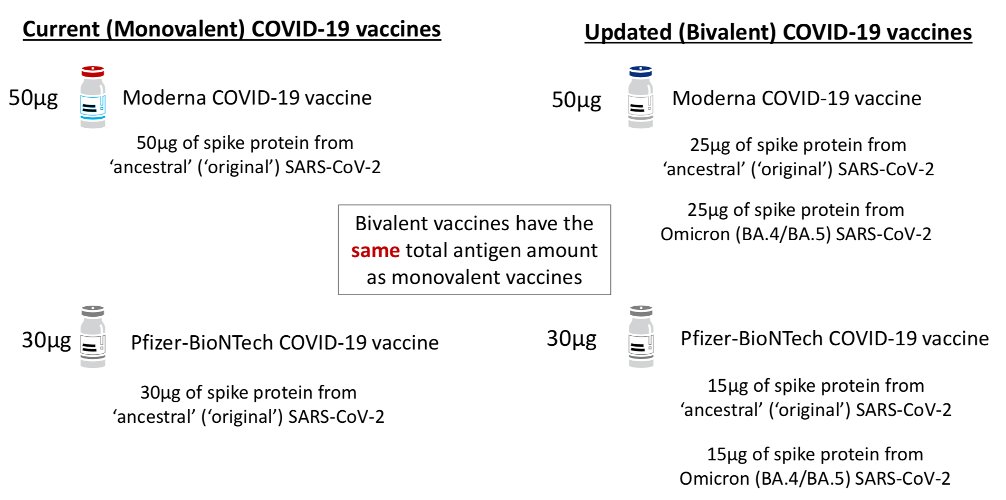
If you have yet to have the initial, two dose COVID vaccine series you will get the original vaccine without the Omicron component. The new vaccines are only for booster shots, and the reason for keeping the original vaccine is not clear. It may be that the lack of full human testing has delayed the replacement of the initial vaccine series.
- Are they safe for people to receive?
Safety appears to be the one definitive thing about these boosters. Since these vaccines are structurally identical to the original mRNA vaccines, local reactions to the shot and generalized reactions, such as fever or feeling ill, should be no different than what has been observed with the prior COVID mRNA vaccines.
Many people have pointed out that these vaccines have not been fully tested in humans. While this is a theoretical concern for safety, it is a similar situation to Flu vaccine, where the vaccines are structurally identical, but contain different antigens corresponding to the virus strains people suspect might be a problem this fall and winter. Given the safety observed in hundreds of millions of people with mRNA COVID vaccines, it is unlikely any new problem will be observed.
- Are these boosters better than the original vaccines?
There are several unknowns about efficacy here.
First, the presumption is that the new boosters will be more effective in preventing Omicron lineage (like) viruses. Data for this comes from studies with a two-component mRNA vaccine containing Wuhan and BA1 (Omicron) mRNA. This is the vaccine that is the approved booster in the EU and was initially intended for the U.S. Studies in humans with this booster showed better antibody responses to all Omicron viruses. But these studies have not been done with the new U.S. boosters in humans. Those were developed to mimic the most recent viruses in the U.S., and as such are too recently developed to be tested in humans.
A comparison of the booster vaccine trials has also shown a slight improvement in the immune response for Omicron containing shots, but an improvement in protection over the original vaccines has not been documented.
All this presumes that any new COVID viruses look antigenically similar to the current Omicron variants that are circulating. Part of the reason that original Wuhan sequences are also present in the new boosters may be to provide broader response just in case a new virus looks more like the original SARS-CoV-2 than omicron. The good news is that several studies have suggested that even using the original booster improves short term protection to infection with all forms of COVID viruses (see below).
- Will they prevent COVID infections?
It is clear now that these vaccines do an excellent job of preventing severe COVID-19 illness and death. This is related to the strong cellular immunity they produce. There also appears to be short term protection against actual COVID infection related to antibody produced from the vaccine. Unfortunately, antibody protection wanes quickly and is gone about six months after the vaccine is administered. Therefore, we can expect benefit from these boosters in preventing COVID infection for at least six months after the vaccine is given.

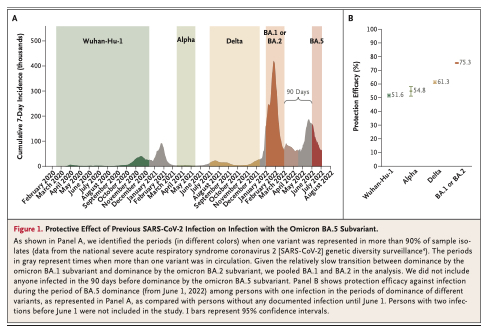
A more important point is that infection itself serves as an effective booster of immunity. As demonstrated below, if you have been infected with any Omicron virus (identified as BA1, BA2, BA4 or BA5) you have strong protection (75% as seen below) against current infection.
How do you know what you were infected with? Basically if you have been infected in 2022, then it was with a form of Omicron virus.
- Who should take them and when?
Anyone over 50 years of age or with significant health problems that might predispose to severe COVID infection should take the booster. You also should be 4-6 months out from your last booster or documented COVID infection otherwise the vaccine may not effectively stimulate your immune system.
- Bonus question? Should people under the age of 18 get these booster vaccines?
Given the lack of efficacy data and the minimal risk from COVID infection in younger people, I don’t think it’s warranted to insist that people below the age of 18 get these booster vaccines at the present time.
Jim,
Thank you for this clear, complete and easy to understand article and punchy, clear illustrations, answering all the key questions about the new booster! This is the best and most thorough explanation I have read, and is sorely missing from the confusing current state of public information about the new booster! Cath
>
LikeLike
Thanks Cath! Jim
LikeLike
I had 2 covid vaccines and 1 booster. I had covid in July. I was told by a nurse at my Dr.’s office that I had no prolonged protection from another covid infection since the current strain is so contagious. She told me they were seeing people reinfected after 2 or 3 weeks after an initial bout of covid. I’m heading to CA in 3 weeks for a family wedding, and am considering getting the current booster. I was told by my Dr. that I can get the new booster. After reading this article, I am reconsidering. Thoughts? (I am 61 years old with no underlying health conditions.)
LikeLike
There is immunity from infection. What wears off quickly is antibody that protects from reinfection.
You are two months out from your infection so you are technically eligible for the booster. It may slightly reduce the likelihood that you will get reinfected depending on what strain you were infected with and what is currently in California.
It is a small benefit and likely you will do well if you get infected regardless.
Hope this helps.
LikeLike