The Internet has been ablaze with stories about a potential COVID-19 surge that is anticipated this winter. While most of the articles strongly argue for the likelihood of a surge, there is no hard data indicating that the United States is indeed going to experience new infection outbreaks. In fact, most areas in the country are currently seeing a decrease in COVID infections as the BA.5 variant wave recedes.
Much of the speculation on a winter wave is based on the discovery of a new variant of the SARS-CoV-2 virus called XBB. While some have called this a “nightmare” virus, it really is not that different from prior COVID-19 viruses. Of interest, bloggers tend to focus on infections and not deaths or serious illness.
One prominent Twitter participant provides an ominous warning that “deaths and hospitalizations are up,” but only provides actual numbers for infections. The full data shows that these more severe outcomes of COVID with the XBB virus remain rare!

In reality, the XBB variant is based on Omicron viruses and has similarity to several prior viruses including BA.2 and BA.5. Many bloggers claim it is more contagious and better able to escape prior immunity induced by infection or vaccine, as well as being resistant to monoclonal antibody therapies such as Evusheld. While the Evusheld concern is likely true, the immune escape seems overblown.
There are credible reports that this variant is causing increased numbers of infections around the globe in places such as Europe and Singapore. However, several features and issues concerning this virus need to be clarified.
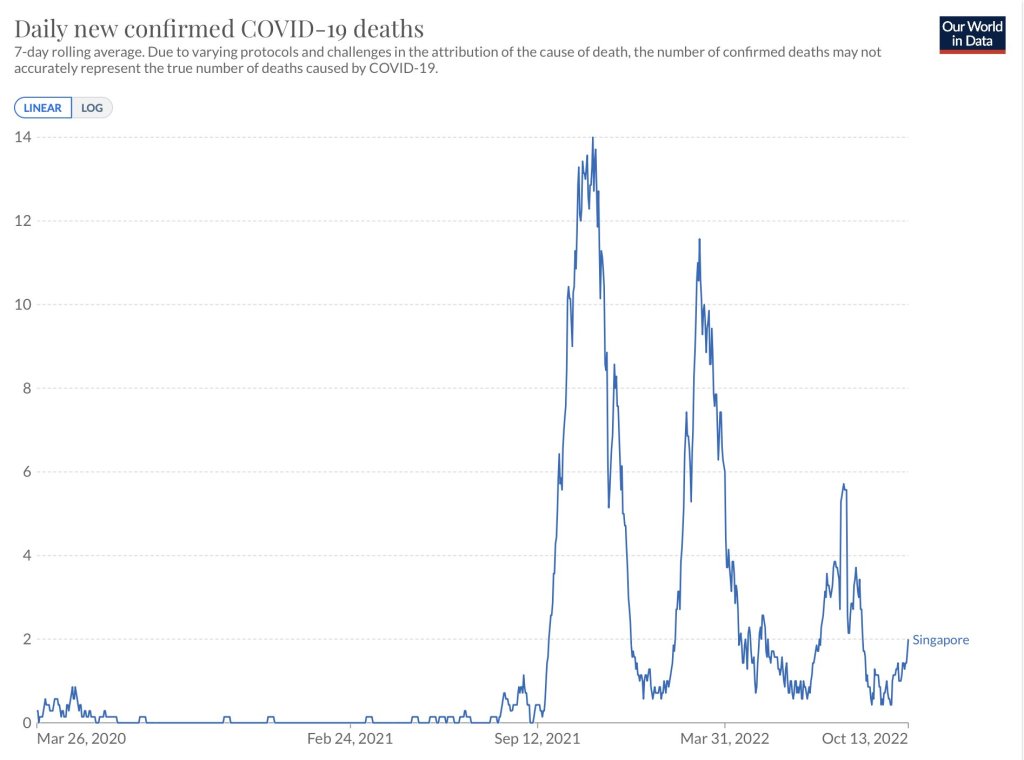
- The claims of this virus being more contagious have not been validated. In fact, increases in infections in places like Singapore mirror prior Omicron waves of COVID.
- While monoclonal antibodies against the virus may not work, antiviral drugs like Paxlovid are very effective in treating infections.
- The current COVID vaccines appear to work well in preventing infection with this variant. In particular, the vaccines appear to provide protection against severe illness.
- Prior infection also seems to give protection against this variant since only 10-15% of all cases are re-infections.
- Overall, serious illnesses and death seem to occur at similar, lower rates as with Omicron variants.
Given this, while there is always the need to prepare for the worst, there is no need to panic right now. A few simple steps can assure you can get through whatever happens with COVID this winter.
- Get the current booster. If you are more than 6 months out from a prior infection or previous booster, get one of the new bivalent vaccines.
- If infected and you are over 60 years of age, or have serious medical conditions, take the Paxlovid antiviral. Also, if you are on other medications, you can work with your physician to decrease or drop these meds as necessary for the 5-day course of the antiviral drug.
- If you get infected, don’t return to the workplace until your nasal (antigen) test is negative. Regardless of what the CDC says, don’t go out until you are negative for virus and cannot spread COVID to anyone else. Also, wear a N95 mask for a few days after returning to work to make sure you don’t infect anyone.
- If you have serious immune problems keep aware of local infection rates and consider staying home when over 10% of individuals in your area are positive for virus.
One thing for sure, with the current tools we have to prevent and treat COVID there is no reason to panic this winter even if you become infected.
Dr. Baker
We are good friends of Genie & Reid Sherard and met you in Ann Arbor. Thank you for a reasoned well explained update on Covid. Thank you and we appreciate your insight and opinions.
Hope to see you here in Charleston!
Greg & Betsy Jones
Sent from my iPad
>
LikeLike
Thank you.
Jim Baker
LikeLike
Hi Jim. I hope you’ve been well. Ive been enjoying reading your blog.
The resistance to Evusheld prophy and, from what I’ve read, treatment of active infection with bebtelovimab, is concerning for our solid organ transplant recipients. The interaction with Paxlovid and tacrolimus can be profound and it’s magnitude and duration unpredictable, so we’ve been strongly advised to use MABs instead.
All the best,
Keith ________________________________
LikeLike
Yes, transplanted patients are probably the most difficult population with this disease outside of lymphomas. Cellular immunity is so very important.
Aside from that I am surprised that the government has not been funding ongoing development of monoclonals. Jim Crowe may be in process for this at Sandy (developed Evusheld).
Best
Jim
LikeLike
My wife came back from France in the last week of Sept and tested positive four days after her return. She suspects she got it on the train to Degaulle Airport or on the flight home. It knocked her out for 3-4 days (she didn’t get a booster before she left in early Sept) and when I tested positive a few days after her, I only had one really bad day – I had the new variant booster two weeks prior. We’re both fine now.
Long story short, if she got one of the “new new” variants in Europe, it was pretty bad without the recent booster, at least in our house (N=2).
LikeLike