I’ve been asked by several readers to evaluate an editorial in the Wall Street Journal with the provocative title “Are vaccines fueling new COVID variants?” This editorial by Allysia Findlay, a non-medical member of the Journal’s editorial board, proposes that vaccinating individuals against COVID-19 is now responsible for driving the creation of new COVID virus variants that are announced every month or two to great fanfare.
More disconcertingly, the editorial seems to suggest that by vaccinating individuals we have in some way crippled our immune system to respond against new versions of the SARS-CoV-2 virus as they emerge. While this editorial has been influential in raising substantial concerns, especially given the ongoing pursuit of new vaccines for COVID, it has fundamental scientific errors that undermine its postulation.
First, it is not vaccines but human immunity that drives virus evolution. The human immune system exists in equilibrium with infectious agents in the environment. It is activated to protect the individual in response to exposure to infectious agents. It also has a memory, so it can respond more rapidly when it sees an infectious agent that it has already encountered. In response, the infectious agent mutates its genes to try and overcome immune protection.
The human immune system cannot provide absolute protection against any pathogen. Immunity does not respond equally well to all infectious agents, and its ability to totally prevent any infection is relatively limited, especially compared to immunity’s ability to eventually destroy and clear infections after they occur. This is because these two actions are mediated by different types of immunity. Antibody immunity provides the rapid neutralization of infectious agents to prevent infection. Cellular immunity provides the long-lived and more effective ability to clear agents once they have infected an individual.
Antibody immunity is more limited than cellular immunity because the way it recognizes foreign materials is very specific. Cellular immunity recognizes smaller components of infectious proteins that are more likely shared between different infectious agents. This wide-ranging ability to recognize related “variant” organisms makes cellular immunity the real key to our long-term survival.
The other problem with human immunity is that each individual’s immune system does not protect against everything. Everybody has holes in their immune system that allow certain types of infections to escape normal immunity. Only 95% of the population responds to even the most effective vaccines, so we can never protect everyone. Nature handles this by giving everyone a slightly different immune system. In this way the ability to recognize infectious agents is unique to each individual and so are the holes in our immunity. As a result, while an infection may escape a few individuals and kill them, overall our species survive.
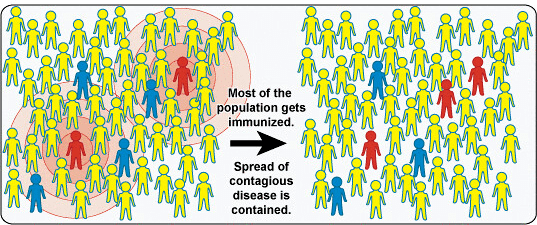
How is it that we were able to develop lifelong vaccines for some infections while other infectious agents like influenza and COVID rapidly escape vaccines? This is not due to inadequate vaccines, but is the direct result of the nature of the infectious agent. Vaccines that provide long-term protection only work with infectious agents that are stable. Most of the viruses for which we have lifelong vaccines involve genetic material that does not rapidly mutate and are therefore provides little opportunity to escape immunity.

In contrast, viruses like influenza, COVID and even HIV are based on RNA genetic material that is constantly mutating. This allows these organisms to continually challenge the immune system with proteins that can escape antibody protection. Importantly, immune escape occurs whether the human immunity is generated from vaccine or prior infection. Therefore, it’s really the nature of the infectious agent that drives variant development rather than vaccines.
The mRNA COVID 19 vaccines have provided us a remarkable way to boost our baseline immunity against COVID 19. This has allowed us to develop herd immunity to SARS-CoV-2 that has ended the horrible pneumonia and rapid deaths that occurred early in the pandemic. While people are still dying when infected with SARS-CoV-2, they are mainly dying with COVID because of another coexistent health problem, rather than from COVID infection. If we were unable to make an effective immune response to the new variants each time a new one emerges, it would look like the first wave of the pandemic, with everyone having serious pneumonias and many people abruptly dying.
Our biggest issue going forward is how often we should boost immunity against SARS-CoV-2 to maintain our cellular immunity without side effects like autoimmunity. It’s clear we should not be chasing every new variant with a new vaccine. These variants come and go within months, and the effort to try to prevent infection by generating antibodies is impossible to maintain. We probably should look at some more reasonable interval between vaccinations that maintains the cellular immunity that keeps people from getting deathly ill from COVID 19, but still makes sense in terms of healthcare impact, feasibility, and costs. This is a decision that public health authorities need to make soon, and it should not be driven by vaccine manufacturers.
In summary, it is inaccurate to claim that vaccines are driving the development of new COVID variants. It is actually the high genetic mutation rate of the RNA COVID 19 coronavirus that leads to the development of variants that escape immunity. This virus will continue to mutate to escape immune protection in order to survive. Blaming vaccines misleads people as to the nature of immunity necessary to control COVID 19 infection and hinders the implementation of a vaccine strategy that’s both practical and effective.
Nice summary, if not a tad wonky (for a general audience).
I suggest you submit it to the WSJ as a rebuttal. Hopefully, to be published in their opinion section instead of some obscure “letters to the editor” section. 🤓
LikeLiked by 2 people
Thanks, Jim. It demonstrates how careful we need to be to believe anything in print. I am disappointed that the WSJ did not “fact check” Findlay’s editorial. I did not bother to read it because it seemed sensational to me and will probably not likely read any other pieces by Findlay in the future.
>
LikeLiked by 2 people
Dr. Baker,
Again, another timely and informative blog on this ongoing health issue. Thank you for the clarity and explanation.
LikeLiked by 2 people