I thought I would end the week on a positive note! Despite the remarkable challenges we are facing there are reasons to be optimistic. Science, circumstances and even natures evolution may combine to make this event managable and something we can learn from for future pandemics. Here are seven reasons why the US could control this outbreak.
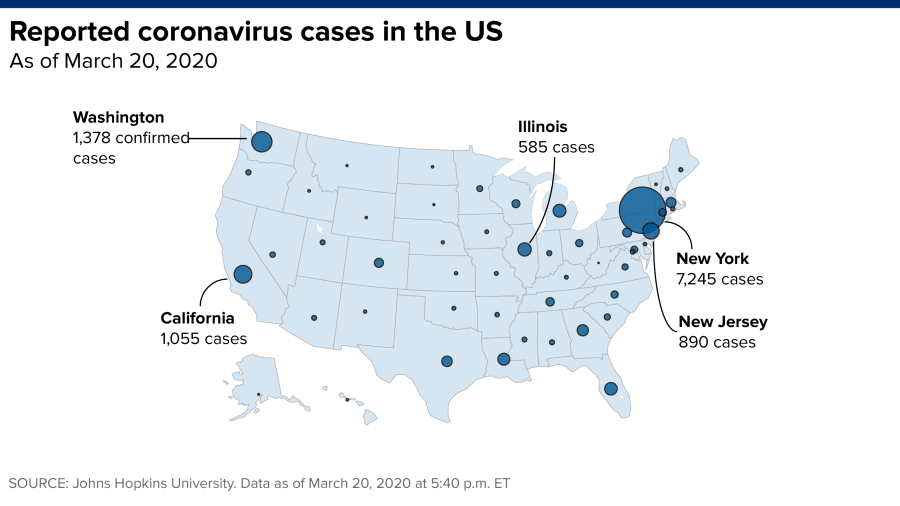
1) Social distancing does work! The biggest problem we face is the huge surge in the number of sick and hospitalized patients from the first wave of the pandemic. Social distancing can prevent this as was shown in Asia, and this could spread out the timing of the infection so that we are able to handle it medically. Stop worrying about testing; it is irrelevant in this situation as EVERYONE should practice the social control measures. This is especially true in places with significant numbers of cases (see Figure 1). If we address this most important problem effectively everything else will be easier.
2) There are probably many more people that have been infected than we thought. I think that there are many more people in the US infected with this virus than was thought, especially given the limited testing and the fact that most people don’t get sick (also the early death rate estimates used to back calculate infection numbers were much too high). That this is a good thing seems paradoxical, but those individuals who were infected and recovered serve an important purpose. Each recovered patient is an individual who can’t get re-infected and cannot spread the infection to others. This concept is called “herd immunity” and has been shown to be valuable with many vaccines. (Figure 2) Thus, if more people have been infected, especially with lower numbers of serious illness, it will blunt the surge.

3) US hospitals have the ability for surge capacity. Hospital infrastructure in the US, despite its shortcomings, is better than in most of the European countries and there is the ability to search intensive care unit beds. As an example, my own University of Michigan Medical system has been able to set up a surge unit with 32 new infection control beds in the pediatric hospital. It has negative pressure rooms and should be effective in treating patients and controlling the infection. Similar efforts are being done in all the major hospital systems across the country. While this pandemic will put extreme pressure on our health systems, they are well organized and have plans defined; the real issue is implementing the plans in a short timeframe and making sure we flatten the surge curve (Figure 3)

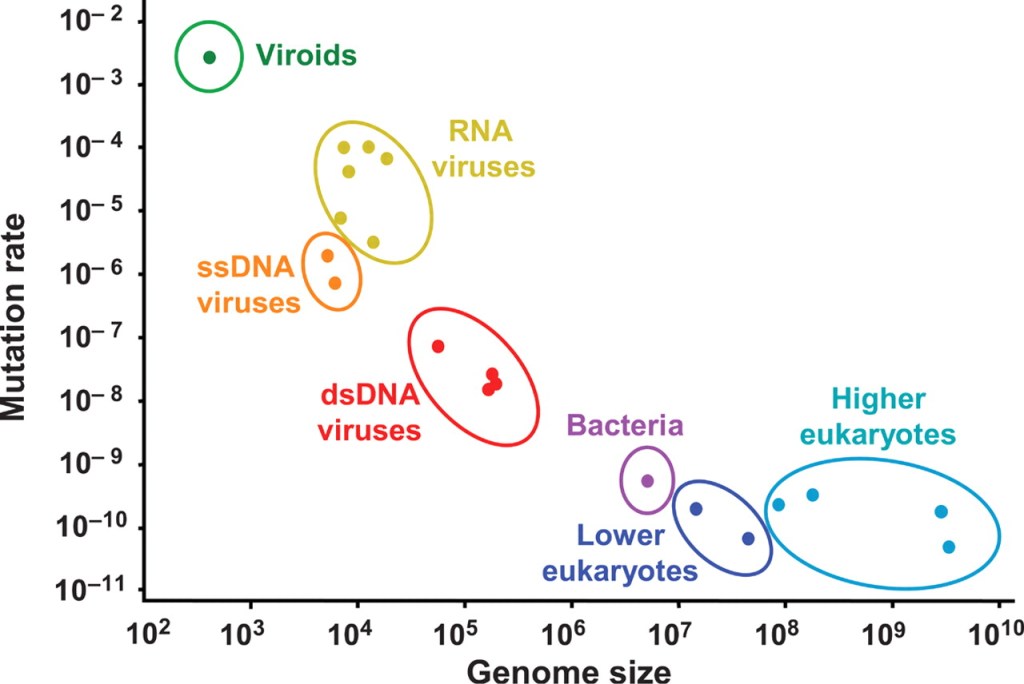
4) Coronavirus is an RNA virus. RNA viruses have a remarkably high tendency to mutate. (Figure 4) Mostly, they mutate towards decreased pathogenicity because this helps the virus; people who have the virus and don’t get sick (or die) are more efficient at transmitting the virus. We already have seen that there are two isotypes of coronavirus circulating; the one that predominates in the US appears to cause less severe disease but is easier to transmit. If the virus continues to mutate it may result in a low-grade infection that works like a vaccine to induce immunity without the mortality.
5) Summer is coming! There is a debate about whether this infection will decrease during the summer as is common for most respiratory illnesses. There are reports that this virus doesn’t spread as effectively in warm and humid climates. However, while most coronavirus infections are seasonal some may have less seasonal variation. Despite this I think it’s likely to see some falloff in cases with warmer weather. This will give us a respite to focus on developing new therapeutics and vaccines.
6) There are a number of anti-viral drugs that could treat this infection. As I stated in my blog on repurposing drugs, there are a number of antiviral drugs that show promise in controlling RNA viruses. Favilavir has already been approved in China based on trials there. Remdesivir is thought to be a strong candidate due to cell and animal studies, and there are many others being considered. Specific anti-inflammatory drugs against IL6 and other causes of inflammation could soon be tested. The key here is that we need to do control trials to make sure that these drugs work and eventually compare their efficacy. The hype around a drug like chloroquine is distracting, as the mechanism of that drug’s action is poorly defined and it has significant toxicity. Regardless, there should be at least two or three antiviral drugs that can treat this infection in the next six months.

7) We are not focused on a vaccine as an immediate intervention. While again this may seem paradoxical, I have personal experience in this regard. Developing a new prophylactic vaccine is very difficult to accomplish. The biggest problem is that the safety threshold is incredibly high. Remember, you will be giving this vaccine to people who are otherwise healthy at a time in the future when (hopefully) coronavirus will be less of an immediate problem. Any toxicity from a vaccine won’t be tolerated. During the 2009 swine flu H1N1 epidemic, a new flu vaccine was developed by GSK using unique immune stimulants. It was later noted to be associated with the subsequent development of narcolepsy (a sleeping sickness). While it is not clear whether this vaccine actually caused narcolepsy or it was another even associated with the infection, it will be difficult to use this vaccine in the future as you cannot induce even a rare, life-threatening side effect in non-dire circumstances. While there won’t be a vaccine soon, for this first wave, this doesn’t mean we should not immediately start on many vaccines (I will be doing a blog post on vaccines for this disease soon).
So, there is reason for optimism, especially if we work hard at preventing the surge, the virus helps us by becoming less deadly, and we get the antiviral drugs we need. The consequences of these events could make this summer a much better time. We must then use the lessons we learned to make drugs and a vaccine to prepare for future and hopefully lesser waves of infection.
Sent from my Sprint Samsung Galaxy S7 edge.
LikeLiked by 2 people
This has been very helpful and encouraging. We will our hopes up and look forward to the blog post.
LikeLiked by 1 person
Thank you so much for sharing this valuable information. We are friends of your buddy, Peter Hillman and his wife Lisa. Alex and Dona Garnett
LikeLiked by 1 person
Thank you Jim. Informed, fact-based reasons for hope are so important right now.
LikeLiked by 1 person
It is most encouraging to be given information that promotes optimism! Thank you.
LikeLike
This has been very helpful. But i expect no less from my good friend. However I don’t think your system is working as I signed up for email notifications when you add new posts.
LikeLike
Goodd reading your post
LikeLiked by 1 person