Executive Summary
- Coronavirus infections need to be self diagnosed
- This can be done by identifying a number of characteristic symptoms
- Individuals who suspect they are infected should contact their physician and not go to an emergency room or hospital
- Anyone with suspected coronavirus infection should self-isolate for 14 days regardless of whether they have had a test for the virus.

We have now entered a phase of the pandemic that our major concern is how to tell if we have a Coronavirus infection (COVID–19) and what to do when you think you are infected. Since the virus is now circulating in our communities we can stop worrying about contact with people from “endemic areas”; we are in an endemic area! Also, as healthcare systems and doctors become increasingly overwhelmed with this disease it may be difficult to get direct physician input. Importantly, if one is concerned about being infected, possibly the worst thing to do is to go to an overwhelmed emergency room that is unlikely to provide care or even a diagnosis. It’s therefore important for each person to determine the likelihood that they are infected and develop an approach about what to do with that concern. Understanding self-diagnosis and the necessity for subsequent medical care will help people cope with the potential of being infected and make it easier to decide how to care for yourself and family members. The CDC has an excellent website on this as well.
This blog is not meant to replace a physician and is not provided as individualized medical advice. If you have any specific questions or concerns please contact your own physician.
How to diagnose a coronavirus infection COVID–19.
At the earliest stages of infection, the symptoms of COVID–19 are similar to symptoms of a cold or the flu (influenza virus infection), and can even be in confused with seasonal allergies. There are, however, some factors that are important to differentiate COVID–19.
Fever; Fever is the most consistent sign of COVID–19 infection. In particular, high fevers in the hundred and 3°F range are certainly not seen with allergies and often not seen with traditional colds, although can be seen with influenza or other viral infections. Having a high fever still unifies a significant disease and is probably the best discriminator for concern of COVID–19.
Cough; Cough is also an important sign of COVID–19. Unlike a bacterial lung infection (pneumonia) the cough with COVID–19 is usually dry and doesn’t produce fluid. The cough can be very persistent and hard to suppress with cough syrup or other medications.
Trouble breathing; The inability to breathe deeply or to expire air consistently is suggestive of a significant lung infection with COVID–19. This is also a symptom that should raise concerns in patients who have underlying heart or lung disease (see below).
Muscle aches; Aching, sore muscles are symptoms of COVID–19 that separated this infection from routine colds and allergies. This symptom, however, is also seen with influenza. Generalized aching particularly in muscles that have not been exercised is a sign of a viral disease.
Runny nose and sore throat; Runny nose and sore throat can be seen but are much less specific for COVID–19. They are usually seen in coronavirus accompanied by a high fever, which is not common for many colds and certainly not observed with allergies.

Intestinal symptoms; Intestinal symptoms are much less common, but can be the first thing seen with COVID-19 and include loss of appetite, diarrhea, vomiting and abdominal pain. These symptoms may worsen as the illness proceeds. It is rare to see coronavirus causing these problems without fever and cough.
A combination of these symptoms, particularly with a high fever and cough, is very suggestive of having coronavirus infection. Given where we are in the pandemic and the suggested public health measures, anyone with these symptoms should presume they are infected and self-isolate for 14 days.
What should you do?
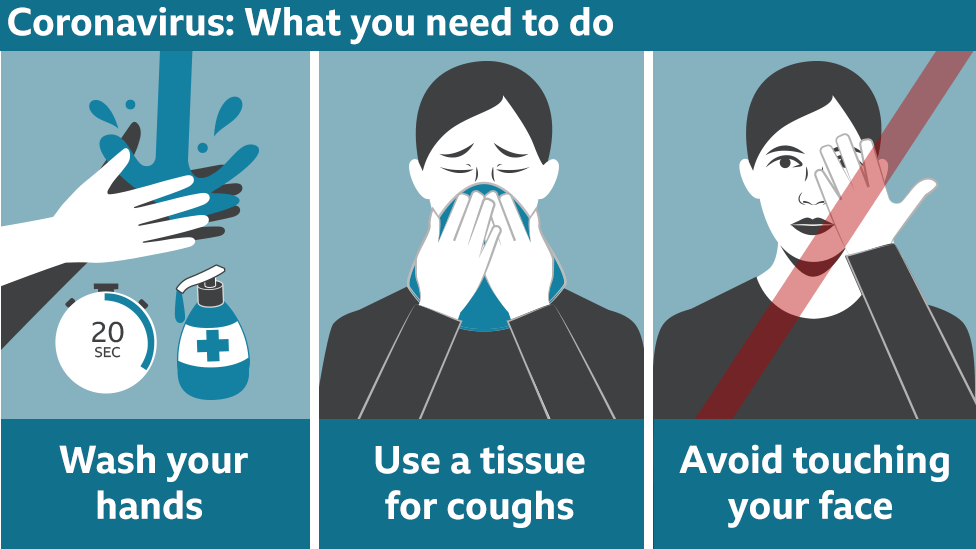
If you presumed you have a COVID–19 infection you do not need a test for the virus unless told so by your doctor. Most importantly, however, you should self-isolate (quarantine). This means stay at home for 14 days and practice control measures. There are several articles describing these measures, but at the very least people with cough or fever should isolate and cover their coughs, sneezes, and runny noses. Vigilant attention needs to be paid to hand-washing and not touching one’s face, and clean surface you and others contact multiple times a day.
You should set up a plan for dealing with the medical complications of this disease. I have set up an algorithm (decision tree) below to help you. This is particularly tailored to our current situation, as the medical system needs potentially infected people to help by deciding themselves what they need. It is important to contact your doctor first and tell she/he that you think you have COVID-19 infection and are self isolating (quarantine). If you have a heart, lung, immune disorder or a muscle disease that makes it hard for you to breath, make sure your doctor knows that and how you are doing. In these cases, your physician may want to get a test to make sure if you are infected. It is best to use a drive through type situation to prevent spreading the infection to others. Otherwise, a test is not necessary and attempting to obtain one will just put you at risk.

If you doctor feels comfortable with your health, it is best to self isolate for 14 days, or as long as your doctor feels is necessary. Again, do not go to the hospital or emergency room unless your doctor tells you.
Take care and stay safe!
It is so great to have this complicated medical issues put in terms that the rest of us can understand. Thanks so much.
LikeLike
This simple video explains coronavirus very well to those without a medical background….
https://ourworldindata.org/kurzgesagt-coronavirus-video
LikeLike
Since many with Corona virus follow advice and likely stay home and recover, I would think estimates of cases world-wide are vastly underestimated. By what multiple?
LikeLike
Well, 35-50% are asymptomatic, another 30% sick but avoid the ER, so maybe underestimate by 60-80%?
Jim
LikeLike