Executive summary
- Rates of infection and death with coronavirus (COVID-19) appear very different in different countries. The reasons for this have been hotly debated. Many pundits have suggested that inadequate virus testing has been responsible due to inadequate isolation of infected individuals.
- Data now show that these differences may relate to who in the population is infected. Countries like Korea and Germany have many more young people infected and therefore have lower death rates. In comparison Italy, where the infection is mainly in the elderly, has much higher death rates.
- Younger people also are more likely to not be ill when infected, and therefore more likely to not be tested and unwittingly transmit the virus.
- Testing at this point in the US is not useful for public health control. Too many people are infected and would be missed by the current test. Instead, everyone needs to social isolate and anyone who is ill with characteristic symptoms needs to presume they are infected.
Much has been made about variations in death rates observed in the current corona virus pandemic in different countries and in different parts of the United States. Some have argued that failures in testing that resulted in a failure to control the infection has caused this discrepancy. They believe that the US, as compared to other countries like Korea, did not identify infectious “carriers” soon enough to stop the spread of the virus. This may not be the case, however, as the differences in deaths persisted over the course of the infection. One variable that could result in these differences is the age of the individual who is infected. Younger people are less likely to die from infection with corona virus and are more often not ill while infected. Therefore, they are much more likely not to be tested and unwittingly transmit the virus.
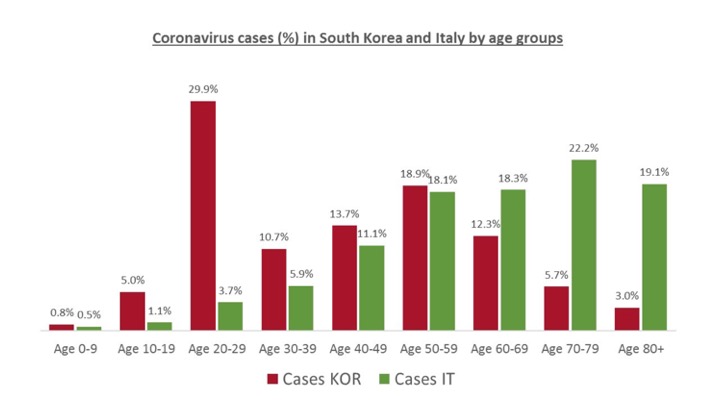
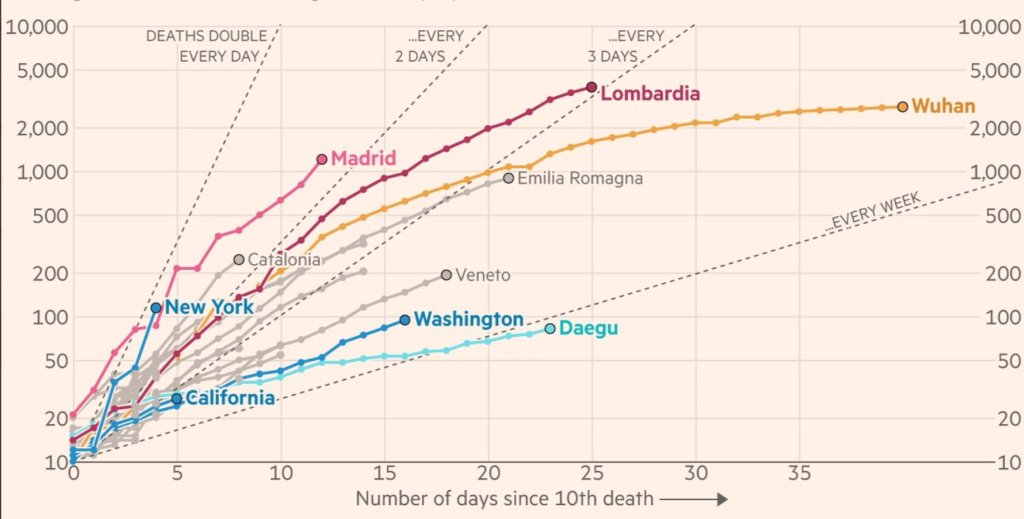
Is there data to support this possibility? People have touted the lower rates of death in Korea are due to their expansive screening program. However, if one looks at Figure 1, Korea has a much younger infected population when compared to Italy. Given the difficulty that older people have in managing this infection, their immune system senescence and other health problems, it is not surprising that Italy would have significant more deaths from coronavirus infection than Korea regardless of testing. Supporting this, the average age of deaths in Italy is 80 years old. Therefore, it would appear that the overriding variable in the severity of illness in these countries is likely to be the age of the infected population. This is also been identified as a reason that Germany’s death rate appears to be lower than the rest of Europe. Death rates are compared in Figure 2 from the Financial Times, and it is interesting that the lower rate in Korea is attributed solely to early screening. The one place where the age of the populations does not explain the death rate is Japan, as they have the oldest population in the world. But there are unique aspects of Japanese society that make it difficult to extrapolate to other countries.

Financial Times @FT.
The same variables also may be important in different locations in the United States. Seattle got off to a fast start in mortality for the reason that many of the deaths came from a single nursing home where a high-density elderly population was infected. New York City (Figure 3) may have similar issues given the high-density of population and the skew towards older individuals. In other areas across the country, the CDC has identified that younger people make up a much larger portion of hospitalized patients, while still experiencing lower rates of mortality. Given the lower rates of significant illness in the young (<50 years of age!), these hospitalizations would suggest that large numbers of well-appearing young people are infected.

Therefore, at this point in time in the US, is there a reason to rapidly expand virus testing as a public health mechanism to identify and isolate infected individuals? This was suggested by Scott Gottlieb, former FDA Commissioner over a month ago, however I believe he would agree that the time for this is well past. Given the current high endemic rates of infection in the US, I strongly support the plan that everyone should practice social isolation. Testing to identify individuals for isolation, since many have no symptoms, will be difficult now even with many more tests being done. The people who are asymptomatic won’t volunteer to be tested, and even with the current testing of sick individuals with appropriate symptoms Dr. Birx reports 90% of people tested are negative for the virus. This clearly shows that testing is a very inefficient means of identifying people who are infected for public health containment!

CloudMinds
What is the current role for corona virus testing in the US if not to control this outbreak? The best use is to help treat sick patients when they present for care. Since we don’t yet have a therapy identified, testing current sick patients is helpful in managing their general care and preventing spread within the hospital. It would also allow enrollment in therapeutic trials for prospective treatments. The most valuable use for testing will come when we have defined, effective therapies to treat coronavirus infection. At that point identifying sick people as infected with coronavirus will allow the early application of therapies for the infection and save lives.
In the long run, it will be important to have a test that shows who has been exposed to the virus that can be run on the entire population. This test will be entirely different from the current one as it will measure immune blood proteins (antibodies) documenting prior/recent infection with the virus (Figure 6). It will be important that this test is highly sensitive and specific (truly identifies who has been infected) so that public health authorities can better understand the dynamics of this pandemic. It will help them prepare for next waves of the pandemic, identifying how many people do not have antibodies and are therefore susceptible to an new infection. This will help define what type of resources will be necessary and even help to identify how we could avoid the next pandemic.
Thank you for doing this Jim. As always, you amaze me!
LikeLike
Bless you good sir…thank you
LikeLike