- Some gave comments that the case fatality rate (CFR) used to calculate the percent of infected individuals in yesterday’s post is too low
- The CFR, which was initially thought to be very high (two people dying for every 100 people infected or 2.0%) has dropped as testing for the virus becomes more widespread.
- With the ongoing, exponential increase in deaths, even if the CFR is higher than given yesterday, it is still likely that 100 million Americans have been infected.
Warning; this post contains quite a bit of technical commentary! I will be back tomorrow with a more approachable post.
I’ve had a fair amount of feedback about yesterday’s post suggesting that up to 30% of the US population has already been infected with CVID-19.
A few individuals were concerned that I was using too low a “case fatality rate“(CFR) or the rate of deaths per number of people infected. Since my calculation worked backwards from that number, if the CFR is significantly higher many fewer people would have be infected.
While the true case fatality rate awaits defining the actual number of the people infected with COVID-19, everywhere that COVID-19 testing has increased the fatality rate has dropped substantially. See the result below from China.

In addition, in the figure below you could see that that country that has tested the most, Iceland, has the lowest case fatality rate. That rate is similar to what was suggested in the post yesterday.
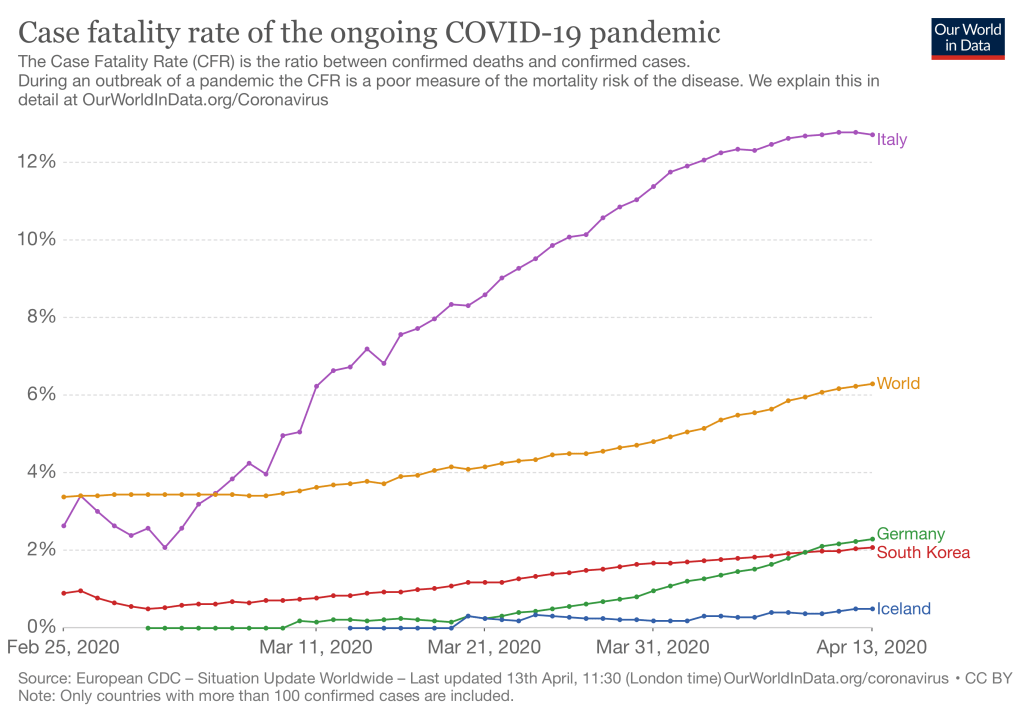
Also, the number of confirmed cases (testing positive) lags behind the number of suspected cases due to low test rates and false negative results from swab tests for virus (PCR). This makes the CFR look higher.
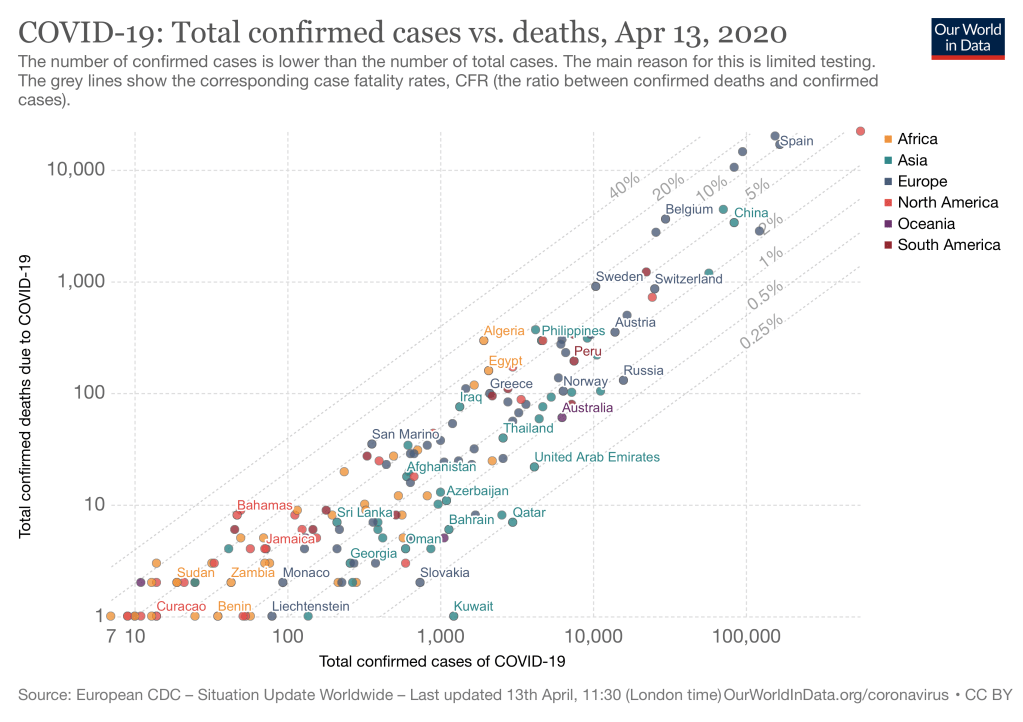
In addition, I received information from Michigan’s outstanding public health school that suggested in February 2020 only 2 of 500 respiratory swabs (PCR) were positive for COVID-19; That would give a rate of PCR positivity of 0.4%. This would be lower than the 1% proposed for the first week of March given in yesterday’s post.
However, anyone who was not ill in February or had minimum symptoms was not tested with respiratory swabs at that time. Also, patients with flu and colds who were being evaluated for respiratory illness diluted out COVID patients. Finally, testing for virus with PCR swabs only identifies the individuals actively shedding virus, not those who were infected (and no longer shedding or those infected but not yet shedding).
Therefore, it is not unreasonable that the infection rate would be about twice the PCR rate, or about 5/500. This is about the 1.0% of the population infected at the first week in March, as suggested in yesterday’s post. Testing has increased tremendously in the past three weeks (see figure below), so catching infected people with the swab (PCR) test for virus should improve.
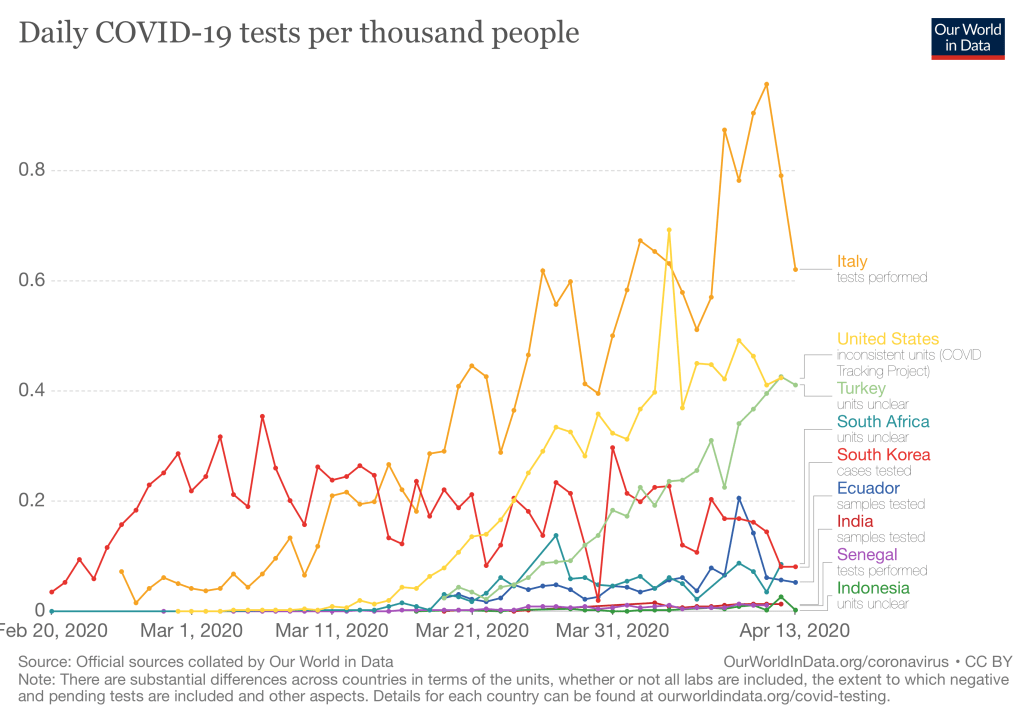
A recent study from Scotland suggested that swab tests (PCR) give numbers of infection 200 times lower than serological rates, especially during exponential phases of a pandemic. This is a finding that will need to be validated elsewhere, but could mean PCR testing has far underestimated the number of infected people. This also isn’t surprising given most individuals have asymptomatic infections.
This study also showed a rapid increase in positive COVID-19 antibody (blood) tests from the 17th to 25th of March. Since the COVID-19 antibody tests only become positive 15 days after infection, it also suggests that there was an exponential increase in infections even earlier.
Finally, since the rate of new deaths in the United States just recently began leveling off, it is likely that exponential rates of infection have existed until recently. Under this scenario even if the CFR is higher, say 1.0% to 2.0%, there would still be 100 million people currently infected int the US.
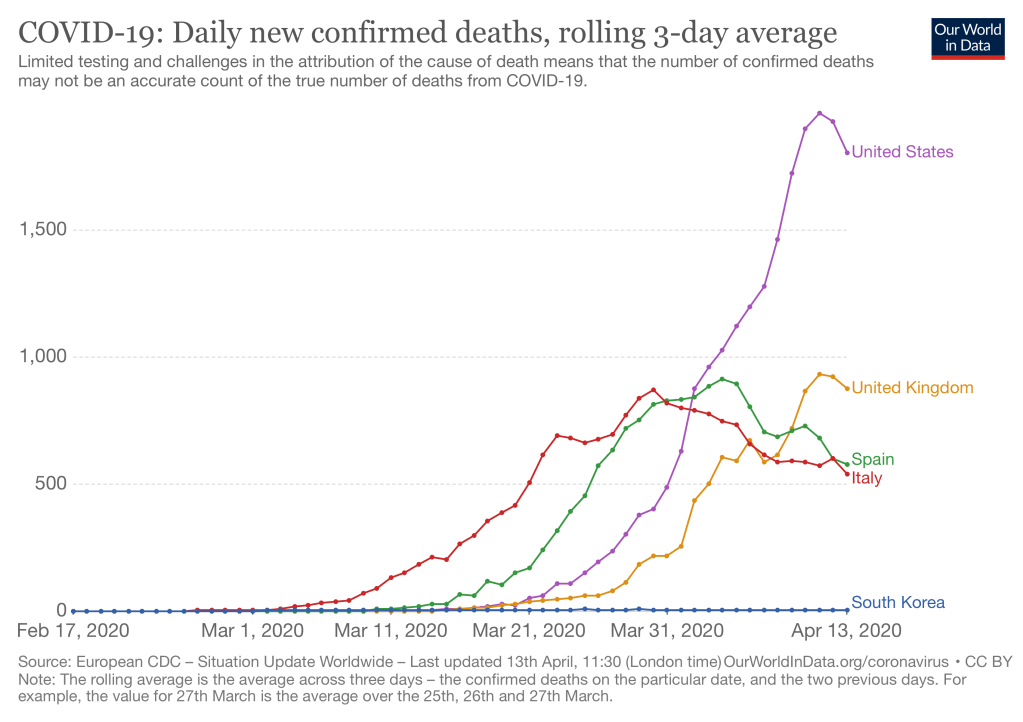
If there is a consensus on any of this, it is on the need to do antibody (blood) testing to determine exactly who was infected. Let’s hope we will be able to start soon.
Thanks for doing this blog. I look forward to every post. It should be highlighted in Ann Arbor News which I find difficult to interpret since it’s numbers and no real perspectives.
LikeLiked by 1 person
Iceland is a bad example. Besides eating a lot of fish, they also supplement their Vitamin D levels with cod liver oil. This 99% white very low poverty population is not representative of the rest of the world, especially those north of about 30 degrees latitude when it comes to ARDS. As the below article points out, cod liver oil sits on their tables in restaurants like ketchup does in the US. Sweden and Denmark do this too; but, they have far more density, racial and socioeconomic disparities and differing immigration policies and populations than Iceland. Perhaps Iceland is a good Covid-19 mortality baseline for what mortality rates could have been in an ideal world where nearly everyone had ideal Vitamin D (and A) levels for their entire lifetimes. It’s not like the world population can start supplementing today and make up for years of deficiencies overnight (but it’s better than nothing) however, once they arrive at the hospital with symptoms of ARDS it’s too late to supplement as dietary Vitamin D supplementation will likely make their pneumonia worse at that point. https://askaboutfood.com/has-iceland-found-the-fountain-of-youth-october-2017/
LikeLike