Reports dominated the news channels tonight about a “new” complication from COVID-19 infection in children — Kawasaki disease. Dramatic pictures of children on ventilators were displayed across the screen with warnings from grieving parents. Since Kawasaki disease is a suspected complication of many viral infections, I wondered what the evidence of this disease was in COVID?
Kawasaki disease is a type of vasculitis (inflammation of the blood vessels). It occurs in children, is usually self-limited, but has a potential serious complication of inflammation caused aneurysms (ballooning) of the arteries that feed the heart. Some physicians believe infections cause this disease, including toxic shock syndrome (which may not be identical).
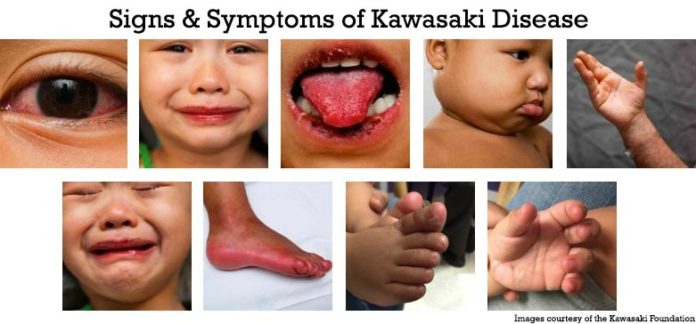
The disease is uncommon, The incidence of the disease in children under the age of 5 is estimated at 8.1 / 100,000 in the United Kingdom, 17.1 / 100,000 in the United States, but is more common in Japan, where it was first identified 112/100,000 (Kawasaki Foundation). It is also thought that Kawasaki is triggered by many types of viral infections, and it has some seasonal occurrence that would support that theory.
While less than 4% of COVID cases are in children and almost all are mild, it still might be possible that the patients contracting COVID-19 develop Kawasaki disease. So, it is worthwhile to examine the data behind this concern. This story seemed to start with unverified reports in the U.K., that were mentioned in passing by The WHO a few days ago.
Today, reports in Forbes Magazine and “The CUT,” focused on the European reports that 12 children have required medical care due to symptoms that were felt to be “linked to the coronavirus.” “Several” of these children were confirmed to have Kawasaki disease. These articles also suggested there were cases in Italy, Spain, Switzerland, Belgium, and France, but the reference for this was a report in today’s New York Times of 15 cases in NYC resembling toxic shock syndrome and/or Kawasaki disease.
After these three stories were published today, the lead was picked up by all major news outlets on the Web and television, and the same claims and quotes were repeated.
The Times article also referred to a bulletin from the state health department stating none of the children died, but most required ICU care and five needed ventilators. The Times also reported “many” of these children also tested positive for COVID-19 virus or antibodies. Overall, only 20 children in the U.S. with COVID-19 have died and most had predisposing illnesses.
So how strong is the medical evidence supporting this association? There is a total of one case report of Kawasaki disease associated with COVID-19.
The Forbes article notes that, “Even though the relationship of this syndrome to COVID-19 is not yet defined, and not all of these cases have tested positive for COVID-19 by either DNA test or serology, New York City’s health commissioner Oxiris Barbot, MD, has asked doctors ‘to report any suspected cases.’ ” In the Times article, which was appropriately titled “15 Children Are Hospitalized With Mysterious Illness Possibly Tied to Covid-19,” New York State health commissioner Howard Zucker said that, “we are following it very closely.” Therefore, the actual association is still under investigation.
In the UK, where this story began, the Kawasaki Disease Foundation released a statement Wednesday, saying that many children with the disease tested negative for COVID-19 and, “there is no current evidence of any increased incidence or greater susceptibility to COVID-19 infection for children who had Kawasaki Disease in the past.” Dr. Liz Whittaker, a member of the Royal College of Pediatrics and Child Health’s allergy, immunology and infectious diseases committee, told the Guardian, “this is not something people should be panicking about.”
Someone should have told the journalists.
Thank you for this column. I had wondered if this was the case. Good to not have to carry around an extra worry about our children.
LikeLike
I agree that the data is distorted when medicine is reported in popular press before evaluation by scientists. And personally, I think that when we are at the point of fifteen case reports, MDs need to be able to freely exchange information without the pressure of outside commentary.
Yet our ER colleagues in NYC have noted many more than “one case”. Last week this seemed like soft data, probable association. This week the numbers are more concerning. Is is mutation? Do we finally have enough numbers to see the rare associations or outcomes? Hard to say. Maybe next week we’ll have better data. But we should not discount concerning symptoms in children, especially in a classic post-viral syndrome, when early treatment of the syndrome prevents morbidity and mortality
And remember (from one month ago!), COVID toes. US knowledge of COVID toes at the beginning of April was zero. Trickles of case reports came in mid-April. Now we know is it a real expression in some children of the post-infectious state. That gain of knowledge was over four weeks of time.
Our understanding of this chameleon virus changes very quickly. Pressure on MDs too early in the epidemic to decide on association or chance is dangerous.
Anyway, here’s what the doctors are saying. As of this week.
EGallagher MD
2020 Health Alert #13:
Pediatric Multi-System Inflammatory Syndrome Potentially Associated with COVID-19
Fifteen cases compatible with multi-system inflammatory syndrome have been identified in children in New York City hospitals.
Characterized by persistent fever and features of Kawasaki disease and/or toxic shock syndrome; abdominal symptoms common
Cases may require intensive care unit admission for cardiac and/or respiratory support
Polymerase chain reaction testing for SARS-CoV-2 may be positive or negative
Early recognition and specialist referral are essential, including to critical care if warranted
Immediately report cases to the New York City Health Department’s Provider Access Line: 866-692-3641
May 4, 2020
Dear Colleagues,
A pediatric multi-system inflammatory syndrome, recently reported by authorities in the United Kingdom,[1] is also being observed among children and young adults in New York City and elsewhere in the United States. Clinical features vary, depending on the affected organ system, but have been noted to include features of Kawasaki disease or features of shock; however, the full spectrum of disease is not yet known. Persistent fever and elevated inflammatory markers (CRP, troponin, etc.) have been seen among affected patients. Patients with this syndrome who have been admitted to pediatric intensive care units (PICUs) have required cardiac and/or respiratory support. Only severe cases may have been recognized at this time.
The NYC Health Department contacted PICUs in NYC during April 29-May 3, 2020 and identified 15 patients aged 2-15 years who had been hospitalized from April 17- May 1, 2020 with illnesses compatible with this syndrome (i.e., typical Kawasaki disease, incomplete Kawasaki disease, and/or shock). All patients had subjective or measured fever and more than half reported rash, abdominal pain, vomiting, or diarrhea. Respiratory symptoms were reported in less than half of these patients. Polymerase chain reaction (PCR) testing for SARS-CoV-2 has been positive (4), negative (10), and initially indeterminate and then negative (1). Six patients with negative testing by PCR were positive by serology. More than half of the reported patients required blood pressure support and five required mechanical ventilation. No fatalities have been reported among these cases.
If the above-described inflammatory syndrome is suspected, pediatricians should immediately refer patients to a specialist in pediatric infectious disease, rheumatology, and/or critical care, as indicated. Early diagnosis and treatment of patients meeting full or partial criteria for Kawasaki disease is critical to preventing end-organ damage and other long-term complications. Patients meeting criteria for Kawasaki disease should be treated with intravenous immunoglobulin and aspirin.
Consistent with the NYC Health Code Article 11, which requires reporting of outbreaks and suspected outbreaks of syndromes of known or unknown etiology and of unusual manifestations of disease of public health interest, any patient who meets the following criteria should immediately be reported to the NYC Health Department by calling the Provider Access Line at 866-692-3641 :
Less than 21 years old, with persistent fever (four or more days), and either incomplete Kawasaki disease, typical Kawasaki disease, and/or toxic shock syndrome-like presentation;
and
No alternative etiology identified that explains the clinical presentation (note: patients should be reported regardless of SARS-CoV-2 PCR test result).
Thank you for your ongoing collaboration.
Sincerely,
Demetre C. Daskalakis, MD, MPH
Deputy Commissioner
Division of Disease Control
New York City Health Department
[1] Pediatric Intensive Care Society. PICS Statement: Increased number of reported cases of novel presentation of multi-system inflammatory disease. April 27, 2020. Available at https://picsociety.uk/wp-content/uploads/2020/04/PICS-statement-re-novel-KD-C19-presentation-v2-27042020.pdf.
Primum non nocere
For more information, send mail to LISTSERV@LISTSERV.BROWN.EDU with the message: info PED-EM-L
The URL for the PED-EM-L Web Page is:
http://listserv.brown.edu/ped-em-l.html
LikeLike
Maybe there is also another virus circulating now. Since some of the children were not positive for COVID, could be that or a co infection or secondly infection. But the press reports not only distort but simplify so doctors stop thinking.
LikeLike
Greetings. I am an avid lay reader of your blog, which I find to be balanced and informative. Could you comment on the recent article by Jeremy Faust, M.D. in the Washington Post on using “excess mortality” as a metric for reopening actions. This seems to make common sense, avoids politics and medical subjectivity (absent testing) but iis evidence based? https://www.washingtonpost.com/opinions/2020/05/04/metric-that-could-tell-us-when-its-safe-reemerge/
I could predict before you reported it that Biscruit was going to drink some Lysol. You have to do a better job monitoring his media consumption. Great blog. Thank you
LikeLike
Did a blog on this. Thank you for the suggestion!
Biscuit appreciates the advice as well (although he is very, very attracted to that Lysol).
LikeLike
My spouse and I absolutely love your blog and find nearly all of your post’s to be exactly what I’m looking for. Does one offer guest writers to write content for you personally? I wouldn’t mind producing a post or elaborating on some of the subjects you write with regards to here. Again, awesome blog!
LikeLike