With all the press about outbreaks in several southern states it has been hard to focus on the exact status of COVID-19 in these places. Several sources are suggesting that the outbreaks are beginning to wane.
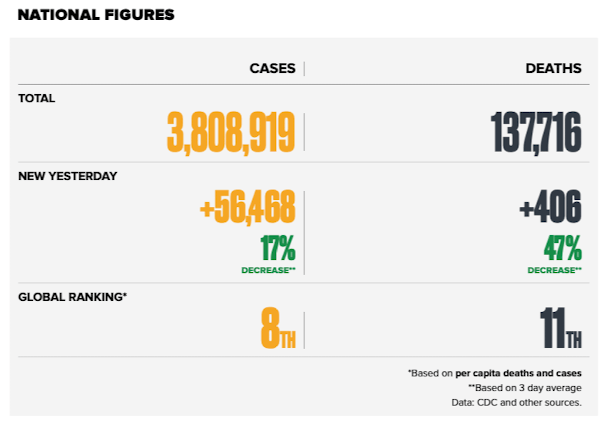
For the third day in a row COVID-19 infections and deaths have decreased in the United States. In a number of southern states where there have been sustained increases in infections over the past month, for the first-time deaths and new infections have stabilized and begun to decrease. Arizona clearly is decreasing while Florida is flattening (deaths are still rising). The exception to this is Texas where the infection numbers continue to rise.
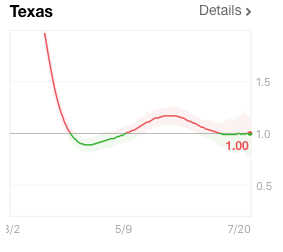
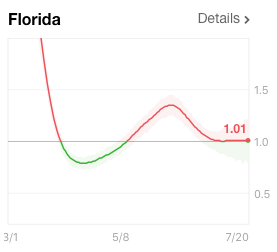
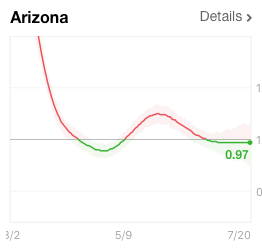
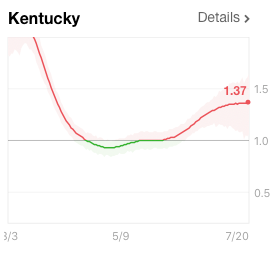
Along with this, the Rt has fallen in most of these states, including Texas. For the first time in a month the Rt is at or below 1.0, suggesting human spread of the virus is starting to contract. The Rt value is essentially the number of people each COVID-19 individual infects. If they infect more than one, the outbreak is increasing. If each person infects less than one, COVID-19 infection is contracting. In contrast to Florida, Texas, and Arizona, Kentucky’s Rt has begun to rise, suggesting a new outbreak in that state.
The reasons that these stabilizations have occurred likely relates to new restrictions on activity, particularly in restaurants and bars. Aggressive efforts to enhance the use of face masks may also be helping. Importantly, the numbers of COVID-19 active and recent infections and individuals with immunity may be so high in some places that there are fewer people to infect. If this follows the pattern seen in the original outbreak areas in April and May, the drop will continue slowly over weeks before control of the outbreak is secured.
It will be interesting to see what happens in Texas, whether they are just earlier in the outbreak and are contracting, or if it is expanding and other factors are involved. It also will be important to see if infections in all these states can be brought totally under control without complete “stay at home orders”. This will help to clarify what approaches would be necessary for handling the inevitable COVID-19 outbreaks we will see in the near future.
Do you really believe that the states are accurately reporting their data? It’s interesting that Arizona and Georgia have such high death rates now even though case numbers are not that high. Maybe it’s easier to obfuscate infection numbers, but deaths are more difficult to hide. also, the country went over 1000 mortalities today for the first time in a while. Makes me suspicious.
LikeLiked by 1 person
No state reports statistics the same way as any other. The real issue is have they been internally consistent, which also hasn’t be always true. Since deaths follow infections I am OK with believing the numbers we are currently seeing out of AZ.
LikeLiked by 1 person
Would love to hear your thoughts on LAMP tests or other daily testing. Why aren’t we rushing these tests to market? Why isn’t the FDA approving? Or are they?
Thank you for your posts. I read them hot off the press – as soon as they show up in my inbox. (I am a food allergy parent that heard you speak some years ago at the NPS / FARE event)
LikeLiked by 1 person
I think eventually LAMP and similar assays that can be done rapidly and frequently (maybe ever 3 days given the dynamics of early covid infection) will be the primary molecular tests. They need to be fully vetted before the introduction though, so we do not get into a mess like the antibody tests where people won’t trust them.
LikeLiked by 1 person
Question: maybe this is dumb, but are we artificially making numbers drop with all the isolation and mask wearing? I know the whole “flatten curve” concept, but what is the end game here? I see unclear discussions on that. At first it was flatten to help our health care providers with an onslaught. Is the idea to gradually turn on the spigot so that we still face the same outcomes but over a longer period of time? If that is so, then aren’t we really just watching the numbers to indicate to “decision makers” when and how to continue to control our interactions?
LikeLiked by 1 person
I think your spigot analogy is a good one. We want to keep a slow, steady flow that is manageable socially and medically. We don’t want a wide open stream that overwhelms health care and social services as was happening in Florida, Arizona and Texas..
LikeLiked by 1 person
Dr. Baker,
Thank you for your Blog! I just watched your podcast on the Michigan Medicine Seminar Series. It was excellent. Hope you do more webinars. I have lots of questions, sorry.
What are your thoughts about monoclonal antibodies? Could this be used to prevent COVID19? I heard the Regeneron REG-COV2 monoclonal antibody cocktail is being studied in hospitalized COVID19 patients and perhaps soon as a preventative- for those who have been exposed to COVID19? If you think this is a viable option, when do think this might be available for those most in need?
I am A-, my husband is O- is there any truth or evidence that I am more likely to have severe symptoms if I got it?
Is Michigan Medicine participating in the Monoclonal Antibody Cocktail or any other studies that may provide some hope for treatment options? I assume Michigan Medicine is already using – Remdesivir, Convalescent plasma, Dexamethasone, and Anticoagulant drugs?
My husband is 70 yrs old- with Comorbidities and I am 60 with Comorbidities. We have been literally in the house-delivery only since Feb 24th. We are waiting and hoping for a vaccine and/or preventative before we will take any risk at all! We miss our 10 Grandchildren- (one of which was born during COVID19) however, we are still unwilling to see or even social distance from anyone due to recent information that as much as 40% of transmission could be from asymptomatic spread. Is there any hope at all that by the end of the year, we could actually go out of the house with a mask on and feel somewhat comfortable? Please we need hope!!!
Thank you for in advance for your reply. I am a patient of Michigan Medicine. I am a HUGE fan!
LikeLike
Don’t know about potential for antibodies yet but data should be coming soon. The blood group difference is minimal, out weighed yesterday other risk factors. UM is doing vaccines and some clinical therapeutic trials. You can check website. Think you can go out with a mask now, not to a bar though. Feeling comfortable is a different thing. Let’s Hope one of the vaccines work. Best. JB
LikeLike