On July 16th I blogged about an article published in the journal Nature showing that cellular immunity to the coronavirus SARS was very long lived. Investigators looked at patients infected with SARS in 2003 and found T cells reactive to SARS present 17 years later in 2020. This was an important finding because it refuted the concept that immunity to COVID-19 was short lived.
Remarkably, this paper also suggested that cellular immunity to SARS could provide cross immunity to COVID-19. This was very interesting but had limited significance since so few people had been infected with SARS and therefore this pre-existing immunity would not help provide herd immunity in the current COVID-19 pandemic.
Today, a paper from the Berlin University Alliance was published in Nature that suggested that T cell immunity to the spike (S) protein of the SARS-CoV-2 virus (that causes COVID-19) was present in individuals who had been infected with the common coronaviruses that cause colds. This would indicate that there is much more potential herd immunity to this infection in the general population than previously suspected.

The investigators were particularly interested in immunity to the S protein because it can mediate protection from COVID-19. In addition, pre-existing immunity might explain the range of symptoms from COVID-19 infection from asymptomatic infection to respiratory failure. Individuals with some immunity could have milder or absent symptoms from infection.
They investigated SARS-CoV-2 spike glycoprotein (S)-reactive CD4+ T cells in the blood of patients with COVID-19 and SARS-CoV-2-unexposed healthy donors. They detected SARS-CoV-2 S-reactive CD4+ T cells in 83% of patients with COVID-19 but also in 35% of healthy donors. This meant that over a third of healthy, uninfected people never exposed to COVID-19 had at least some immunity to the virus.
Not surprisingly the S-reactive CD4+ T cells in healthy donors reacted primarily to the carboxy end of the S protein, which shared similar amino acid sequences with spike glycoproteins of the human endemic, cold-causing coronaviruses. S-reactive T cell lines generated from SARS-CoV-2-naive healthy donors responded similarly to C-terminal S of human endemic coronaviruses 229E and OC43 and SARS-CoV-2, demonstrating the presence of S-cross-reactive T cells, probably generated during past encounters with cold causing coronaviruses. There were also antibodies against all of the viruses, suggesting cross-reactive immunity.

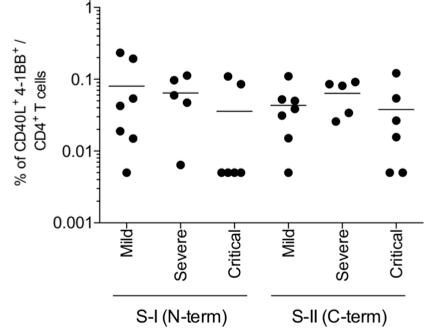
While the investigators looked for associations between pre-existing SARS-CoV-2 cross-reactive T cells for clinical outcomes, they had too few individuals to see if there was an association. However, they believe the presence of S-cross-reactive T cells in a sizable fraction of the general population may affect the dynamics of the current pandemic. If we are boosting immunity in most people, COVID-19 vaccines should also be more effective.
In other words, since 35% of the population has T cells immunity to SARS-CoV-2, we may be starting out half way to herd immunity!

Would it be accurate to say that those not exposed to COVID-19 may have SOME immunity by the coronavirus “colds” we have gotten past, and that is possibly why the majority of folks that get COVID-19 don’t get severe cases? From partial immunity?
LikeLiked by 1 person
Maybe, but immunity that recognizes specific proteins may be enough to turn the tide. Certainly could be responsible for asymptotic infections. Need bigger studies in places like Florida.
LikeLike