I have received a number of inquiries from people who’ve identified a recent article suggesting that a supercomputer has identified Bradykinin as the central mediator of inflammatory disease associated with COVID-19. I have to say that I’m not impressed by this hypothesis.
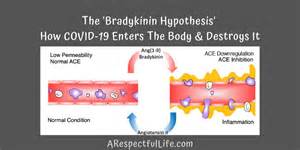
This theory proposes that a single molecule, bradykinin, which is involved in opening pores in blood vessels, causes the severe illness associated with COVID-19. This mediator can also cause leaking of fluid into the lung. A supercomputer analysis of illness from COVID-19 patients suggested this compound might be central to the disease process.
Identifying a single mediator as the center of the complex inflammatory process observed with COVID-19 is probably too simplistic a way to look at this process even though it comes from a supercomputer!
The problems with too narrow a focus has been demonstrated by the analyses that suggested another inflammatory mediator, interleukin 6 (IL6), was central to the cytokine storm that plagues patients with severe Covid-19 infection. Based on this hypothesis, several studies were started with IL6 inhibitors. All of these studies found that there was no benefit to blocking IL 6 in patients with COVID-19. This shows how too narrow a focus can lead investigators astray.

I suppose the good news is that there are approved drugs that block bradykinin action, so this hypothesis can be quickly tested.
As a counter point, another recently published report suggested the more severe cases of COVID-19 were due to suppressive effects on immunity from the virus. This manuscript published in the prestigious Journal of Clinical Investigation suggested that contrary to concerns that there was too much inflammation with COVID-19, it appeared there was too little protective immunity. This failure of host protective immunity then results in unrestrained viral dissemination and organ injury.
Supporting this hypothesis, the investigators used the ELISpot, a highly sensitive, functional assay for evidence of protective immunity. This test was employed in 27 patients with COVID-19, 51 patients with sepsis, 18 critically ill but non-septic patients, and 27 healthy control volunteers to evaluate adaptive and innate immune status by quantitating T cell activity. Circulating T cells, the master regulators of anti-viral immunity, were profoundly reduced in COVID-19 patients. The patients with COVID-19 also produced fewer immune cytokines than observed in septic and other ill patients, consistent with markedly impaired cellular immunity to COVID-19.
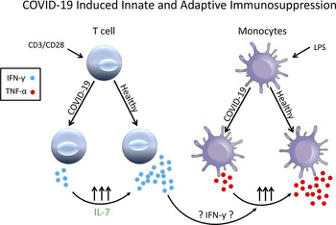
In contrast to the bradykinin hypothesis, these findings support the idea that COVID-19 suppresses immunity allowing the virus to overwhelm infected patients. Strategies to improve immunity in severely ill, COVID-19 infected patients therefore make sense and also seem logical since most patients who are ill with the virus have immune problems or illnesses like diabetes that can suppress immunity.