Where are we at with COVID-19 right now, and why is there such a variety of messages being communicated?
We are in an unfamiliar situation with COVID-19 in the United States. There have been many headlines about reaching new heights in daily hospitalizations and deaths from this third peak of infections. These are all true. In contrast, hospitalization and death rates are proportionately lower than in the spring. I will try to explain the dichotomy of these two realities.
As compared to April, many more people in the United States are currently infected with COVID-19. While some have tried to dismiss this high number of infections as a phenomenon of increased virus screening, what is apparent is that COVID-19 infections are massively higher and more dispersed throughout the population and the U.S. geography than they were early on in the pandemic in March, April, and May.
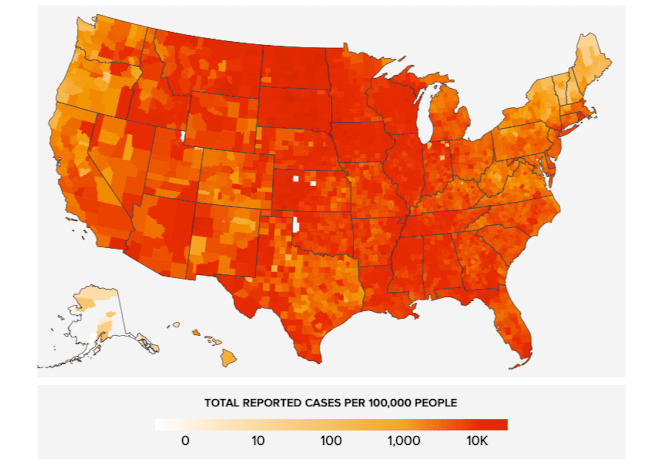
The virus is truly endemic in the population. Everyone knows a close friend, associate, or family member who is or has been infected. Random testing for COVID-19 in symptomatic patients across the U.S. is now positive about 10-15% of the time!
If infections in April had been as widespread as they are now, the health care system would have been totally disrupted because there were much higher percentages of seriously ill COVID-19 patients who needed ICU care. Fortunately, we are much better at caring for COVID-19 patients right now, and younger people are becoming infected, so fewer patients are hospitalized, and those individuals do not need care in the ICU.
Thus, even with lower rates of hospitalization, hospital admissions and deaths have finally reached the point where they’ve passed the numbers seen in the spring simply due to the massive number of infections.
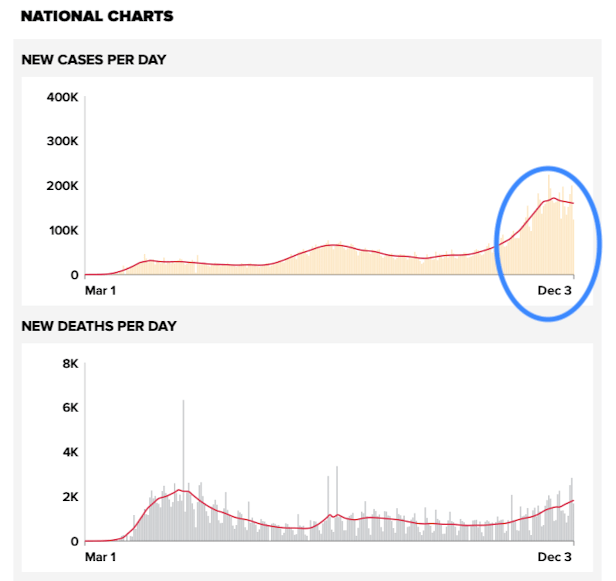
Of interest, the number of new infections in this third peak has actually stabilized and has trended downward over the past week. While this is reassuring, the number of infected people is so high that individuals with severe disease persist in very high numbers. The only thing that will change this would be our efforts to reduce viral transmission over the coming weeks. We also need to remember that we are likely working against a bump in the number of infected people from interactions during the Thanksgiving holiday.
My colleagues in hospital practice report that most of the hospitalized COVID-19 patients are not as ill as they were in the spring, but still require significant care in standard hospital settings. If more of these patients arrive in the next few weeks, hospitals could still be overwhelmed. This will likely happen if the prevalence of infection in the population remains this elevated.
What can we do?
Local officials are already issuing “shelter in place” orders in areas like California where COVID-19 infections are overwhelming the health care system. Many health care settings in a range of states are reducing elective procedures and appointments to save hospital space for COVID-19 admissions. More social restrictions and general, limited health care access are likely in the short term.
Clearly, the long-term answer is that everyone gets the vaccine. But we need to keep our health care system (that has been stressed for months) together until the vaccinations work their magic.
Short term pain for long term gain. Everybody, please, hang in there.