As we try to understand the course of the COVID-19 pandemic, it might be useful to analyze the course of the 1918 influenza pandemic, the closest similar event for which we have accurate public health records.
There are interesting parallels and some important differences between what happened in 1918 and the COVID-19 pandemic of the last three years. Comparing these two events gives perspective on where we are with COVID-19 today and provides insights into the impact that advances in medical technology had on our current situation. (I draw heavily on the CDC’s website for the 1918 information which you can refer to for a more in-depth discussion).
It is hard to evaluate infections in 1918 since diagnostic tests for influenza did not exist. Even symptomatic infections were poorly documented. Therefore, the best comparators are U.S. and worldwide deaths that occurred in both pandemics.
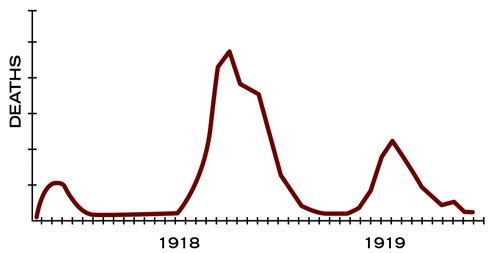
Deaths in the flu pandemic of 1918 occurred in three major waves: the first in the spring of 1918, the second in late summer of that year, and the final wave in the late winter of 1919. By the end of summer in 1919, the illnesses had substantially resolved and deaths that were attributed to the pandemic were thought to end.
The interesting finding from 1918 was that deaths in the second wave were greater than in the first, and much lower in the third wave. Some believed this was because the virus became more contagious during the second wave or more deadly, but it may simply be due to the dynamics of spread. There were no international flights that quickly spread the virus, and a large percent of the infections were spread through troop movements following the First World War.
What’s clear is that after several waves of the 1918 pandemic people stopped dying from influenza. There is no hard evidence that the virus changed dramatically during that time, and since there was no vaccine it is thought that immunity generated by infection was the primary reason that deaths from the pandemic ended.
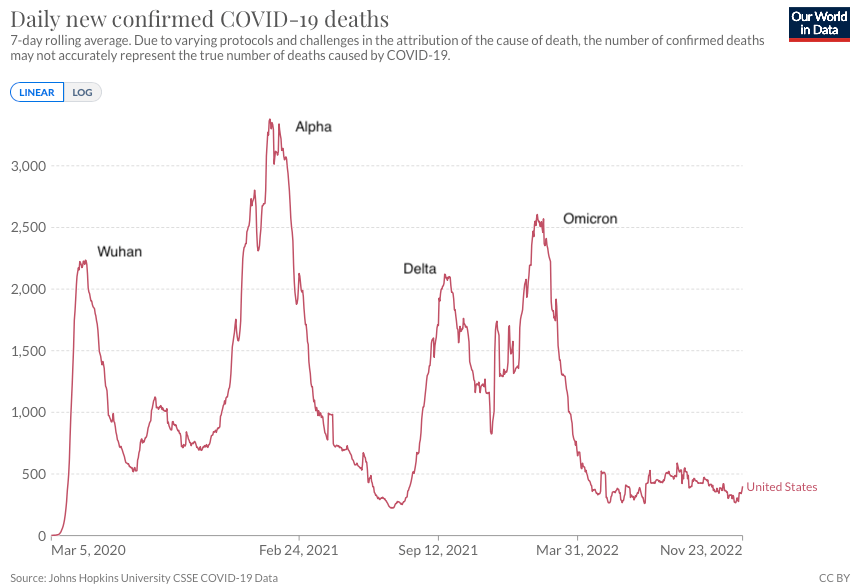
When comparing to COVID-19, the three waves in 1918 can be juxtaposed to the initial (Wuhan) wave, the Alpha wave, and then the binary Delta and Omicron waves of the current COVID-19 pandemic. The Wuhan and Alpha waves spread aggressively in our population without immunity and killed many at risk people with predisposing illnesses. The Delta wave was equally murderous, occurring in the summer about six months after the initial wave, and was closely followed by the Omicron waves that were highly infectious but resulted in fewer deaths. Despite evidence of massive numbers of infections, the number of deaths actually fell, and this suggested either a fundamental change in the pathogenicity of the virus or the effect of background immunity from vaccines and prior infections.
So, did vaccines and new technology help us during the current pandemic? An interesting fact is that in 1918, roughly 1/3 of the world’s population, about 600M people, were thought to have been infected with influenza, which is only slightly less than the number (644M) of people now thought to be infected with SARS CoV-2. However, approximately 60M people died from influenza, and only 6.6 million have died from COVID-19, a 90% difference.
It also is interesting that low level deaths continue to occur from COVID-19 although a wave is nowhere in sight. These deaths could be in older or immunocompromised individuals, a population not present in 1918, or simply identified by better surveillance of ongoing illness. Unvaccinated individuals who have no prior immunity from infection may also account for some of these deaths when they are finally infected.
Given the lack of benefit seen from supportive care (including ventilators) during the first wave of COVID-19, it is clear now that vaccines and the antiviral drugs resulted in significant reductions of mortality from this infection. While the overall reduction vs. 1918 influenza may not be 90%, due to differences in mortality from these viruses, I think everyone would agree that these interventions saved lives. Bottom line; we have made significant progress in medical care since 1918!
Moving forward, our expertise in diagnostic tests will allow us to identify new waves of COVID-19 infection. The observation that deaths dropped precipitously after three to four waves of infection in both the current and 1918 pandemics suggests that future waves of COVID-19 will not cause the deaths seen in the first years of the current pandemic.
Interesting. My grandfather was a epic intern in Vienna in 1919-20, I remember his stories about it.
The longer term epidemiology is still missing Re Covid-19, correct? This remains my major concern (unknown unknowns) re being too cavalier about the non lethal aspects.
LikeLiked by 1 person
Thanks, Jim. Very interesting analysis a and comparison of the two pandemics.
LikeLiked by 1 person
Thank you for continuing to educate us. I appreciate that your column is easy to read and understand while giving data that supports your position.
LikeLiked by 1 person