The headlines today highlighted increases in COVID-19 infections in several states. Of interest, these increases were significant enough to increase hospitalizations, and in the case of Florida, reintroduce social distancing measures. The overall number of daily SARS-CoV-2 virus infections has been increasing slowly since June 1st, however almost all of the increase is related to increases in the states of Texas, Arizona, Florida, and California (as is shown in this illustration from the Wall Street Journal).
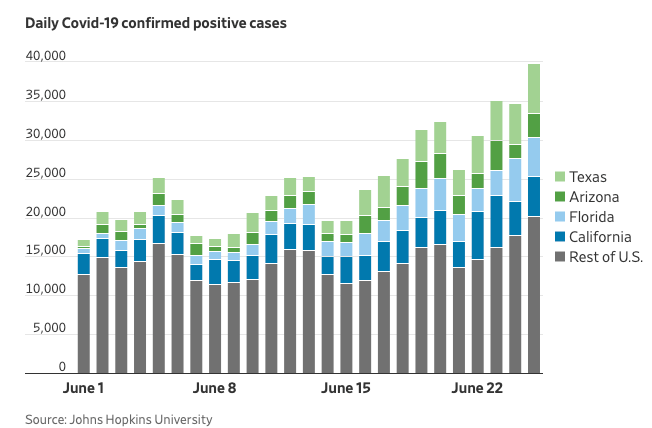
Despite this, the overall number of infections and deaths in the United States has dropped significantly and plateaued from the numbers seen early this year, as shown in data from the IHME
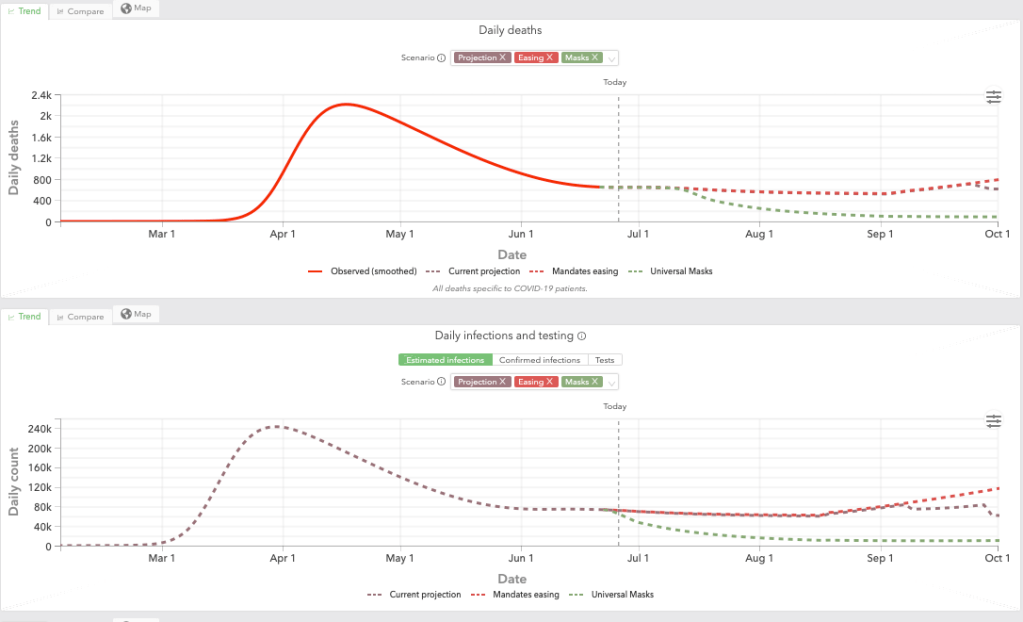
So, what is happening here? Some people have called this the “second wave” of COVID-19, which doesn’t appear correct since it doesn’t seem to be uniform across the country. Dr. Fauci called this a “continuation of the first wave,” which seems to be more accurate. But I believe that much like the “first wave” we are not seeing a wave at all. What we’re seeing are clusters of activity in localized areas. Hotspots of viral activity bubble up, particularly in crowded urban areas, and ignite infections that seem to stay in cities. This is very similar to what was seen initially in places like New York, New Jersey, Detroit, and New Orleans.
In fact, almost every state that had an earlier outbreak is now showing marked reductions of infections. This is shown in this illustration from Johns Hopkins.

Also, even in states like Michigan that are reported to have slight increases in the number of cases of coronavirus infection, the number of deaths has markedly decreased. This suggests that even with infections increasing we are more effective in protecting individuals at highest risk for death from COVID-19.
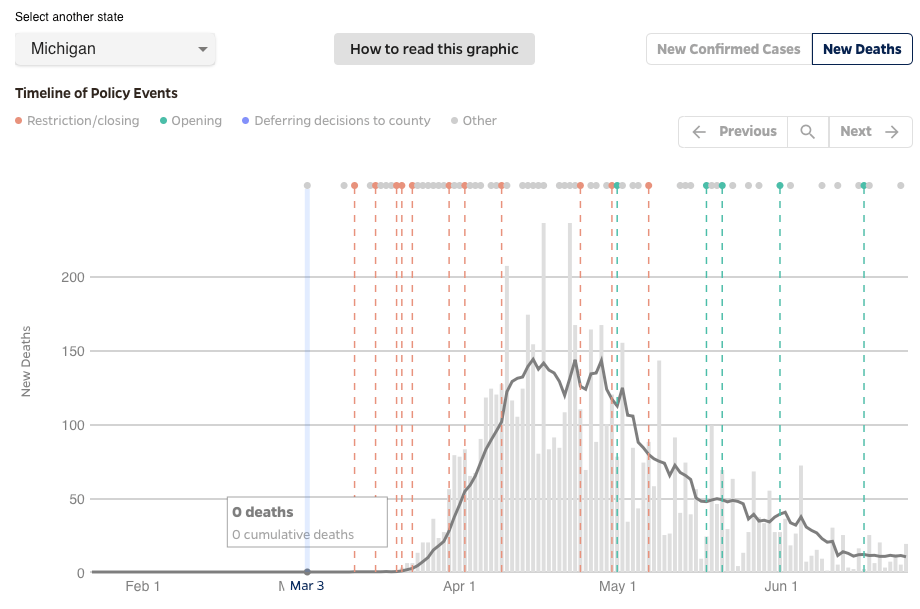
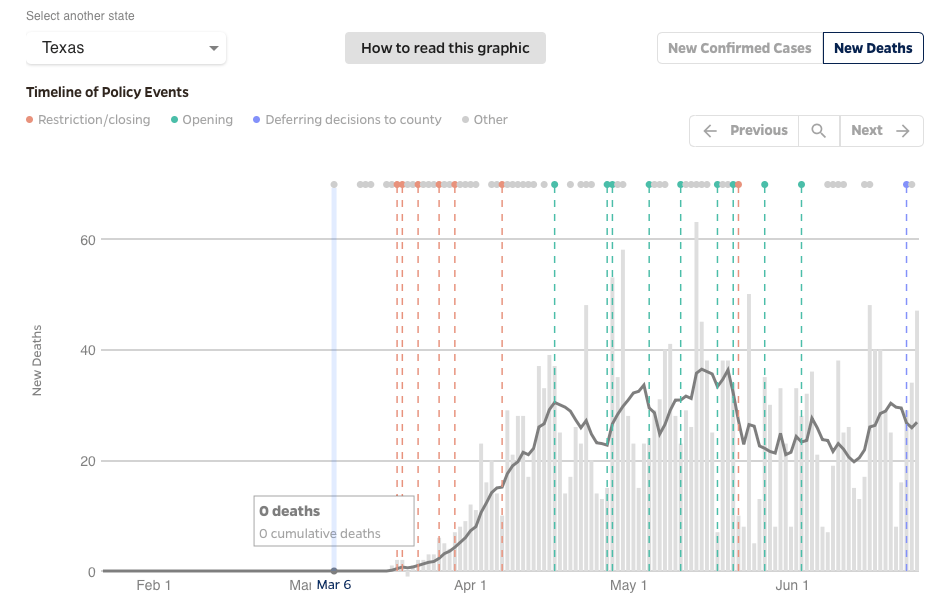
More remarkably, in the states that show the greatest increases in coronavirus cases overall, daily deaths are plateaued or dropping. This may be most closely related to the finding that the new infections are predominantly in young people. For example, the average age of infection in Florida has dropped from 65 to 30 years.
I believe there are several take home messages from this data. First, there is no wave with coronavirus. Infections have not disappeared during the summer and therefore it is not seasonal and unlikely to appear in an exaggerated outbreak in the fall or winter.
In addition, we seem to be better at protecting those who are at high risk of dying from SARS-CoV-2 infection given the reductions in mortality. We need to work hard at improving our care for those individuals to bring down our death rates even further.
Finally, we know what public health tools can be used to reduce infections and control outbreaks. This will prevent overwhelming the health care system.
If we manage these cluster outbreaks and reduce mortality, we should be able to more normally live our lives with COVID-19.


I know your primary concern is to keep us abreast of Covid-19 news, but I’m curious about our regular old flu season coming up this fall and winter. Has a new vaccine been developed for that so it will be available as usual? Perhaps masks and social distancing will make the flu less worrisome this year. I still want a shot, though!
LikeLiked by 1 person
The new vaccine has been formulated and should be take. We can hope that the protective measures will dampen the flu season as they did with the end of the season last spring. Agree with you that we need to take every precaution.
LikeLike
Thanks for bringing some sunshine to the issue. Great to have an informed, unbiased news source.
LikeLiked by 1 person
Think Houston and Miami are probably “major urban centers,” but we will have to watch and wait. Of interest most people that died were not helped by hospitalization, as >85% of people placed on ventilators did not survive. We can hope that remdesivir or other learnings will improve that.
LikeLike